Diabetes is a chronic disease characterized by absolute or relative insulin deficiency due to insufficient secretion and/or action.1 The resulting metabolic abnormalities, such as hyperglycemia, lipid and protein metabolism disorders, contribute to cardiovascular complications, retinopathy, nephropathy and neuropathy.2 Suboptimal glycemic control in diabetic patients has serious repercussions of even more complications, higher cost of care and increased need for services.3,4 Meanwhile, adequate glycemic control prevents acute complications and reduces the risk of long-term complications, the use of services and associated costs.5,6 In clinical practice, achieving good glycemic control for a diabetic patient over the long term represents a challenge. This is because of the complex interplay of the disease process itself, the inadequacy of therapeutic regimens and the attitudes of both patients and doctors.7
In Haiti, the prevalence of diabetes in 2016, according to the WHO, was 6.9%.8 On average, 75 diabetic patients were seen at the clinic every month in 2021 and 80 in 2020 at Saint-Nicolas Hospital for routine visits. They represent about 15% of the clinic, and long-term management can potentially be difficult for the patient and providers. No study to date has been carried out on diabetic patients and the factors that may be linked to poor glycemic control in Haiti.
Considering that 60% of diabetic patients have poor glycemic control,9 this study aimed to identify factors related to poor glycemic control in diabetic patients in an outpatient clinic, having demonstrated above the potential benefits of controlled glycemia. Efforts could be more targeted, and social measures, among others, could be adopted.
METHODS
Selection and description of participants
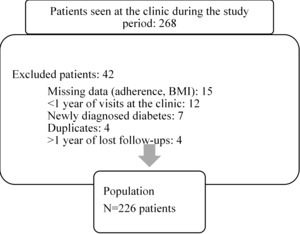
We conducted an analytical cross-sectional study at Saint-Nicolas Hospital in Saint-Marc, Haiti, over three months (March to May 2022.) All diabetic patients seen at the clinic during the study period for their routine consultation were asked to participate. We excluded patients enrolled less than a year at the clinic and patients newly diagnosed with diabetes because we wanted to give them enough time to get used to the routine of chronic disease care and adherence. Patients with more than a year of lost follow-up have to follow up with mental health and are also excluded.
We used a study questionnaire containing the demographic, clinical data, and adherence retrieved from our literature review and the Morisky Medical Adherence Scale -8 (MMAS-8) (Online Supplementary Document). The examiner interviewed the patients (to collect the data in the questionnaires) after each consultation. Training was provided prior to the start of the study by the investigators.
Technical information
The patients were briefed about the study before consultation, and the interview was conducted after their medical consultation. After signing the consent form, their vitals were taken, and they were asked to submit a urine specimen for dipstick analysis. The results for proteinuria were noted in the study questionnaire. Blood sugar level was assessed with a glucose meter used in the clinic. The variables were chosen according to our literature review. 200 patients would provide significant power to detect an effect. The following formula gives the calculation of the sample size:
\[n = \frac{z^2_{1-\alpha/2}P(1-P)}{d^2}\]
P: estimate of the proportion (50%)
D: margin of error (5%)
Z: value corresponding to a confidence level of 90%
We found that the minimum sample was n= (1.645*2 x 0.5 x 0.5) / (0.05*2) = 271. Assuming a non-response rate of 10%, the final size of the sample was n=271 + 271*0.10 = 298.
Poor glycemic control was defined as a fasting blood glucose <80 mg/dl or >130 mg/dl or a postprandial blood glucose >180 mg/dl.10 The relationship between the outcome - poor glycemic control – was assessed in relation to sex, age, duration of diagnosis, blood pressure, presence of comorbidities, employment, level of education, dipstick proteinuria, BMI, dyslipidemia, days of physical activities, medication, adherence (assessed by MMAS-8), visits and HBA1C level.
Uncontrolled hypertension was defined as blood pressure >140/90 mm hg taken on the day of the consultation in a patient with known hypertension. BMI was also defined based on the findings on the day of consultation. Patients answered questions about the duration of their diagnosis, employment, number of days spent engaging in physical activity, and level of education when asked by the interviewer. Comorbidities, medication, number of visits to the clinic during the year, and type of diabetes were noted as found on the patient’s medical file. Dyslipidemia was defined as HDL<45 mg/dl, total cholesterol >200mg/dl or triglycerides >150 mg/dl and was discarded if they were more than 1 year old. Pathological proteinuria was defined as ≥+1 on the dipstick specimen collected.11 HbA1C was discarded if it was more than 3 months old and was defined as abnormal if > 7%.10 Adherence was assessed by the MMAS-8, which has good validity (α=.83),12 and has been used in clinical trials for chronic diseases like hypertension.13,14
Statistics
Data analysis was performed using Epi Info 7.2.2.6 software. We used the presence of poor glycemic control as the dependent variable and the other variables – dichotomized as planned based on the study protocol, available upon request– as independent variables. The analysis included descriptive, bivariate and multivariate logistic regression. We used the odds ratio with corresponding 95% confidence intervals to assess the direction of the association. P value <0.05 was considered statistically significant.
RESULTS
During the study period, we interviewed 268 diabetic patients at the clinic, which was reduced to 226 after consideration of the inclusion and exclusion criteria. With a mean age of 60 ±9.87, most participants were female (84.96%). More than half of the patients, 59.29%, had lived with their diagnosis for at least 5 years, and 67.26% had poor glycemic control. According to the MMAS-8, 50.88% had good adherence.
A total of 202 (89.38%) had at least one comorbidity associated with diabetes: among these 202 patients, 192 (95.04%) had hypertension, including 114 (56.43%) with hypertension alone and 78 (38.61%) with hypertension and at least one other comorbidity. Two-thirds were obese or overweight (59.73%) and less than half had dyslipidemia (42.54%), two considerable comorbidities in our population. Nearly 71% of patients do not engage in physical activities or do so less than 3 days a week. Most patients (70.8%) were placed on oral hypoglycemic drugs, 19.47% received oral hypoglycemic drugs and insulin treatment, and 9.73% received only insulin. Pathological proteinuria was found in 27.42% of patients. Glycated hemoglobin was found in 60 (26.55%) records, half of which were abnormal, i.e., HbA1C >7%. Among the 226 patients, 33.63% were uneducated, 45.13% had a primary level, 21.34% had a high-level education (secondary or university), and 53.98% were unemployed (Table 1).
Patients receiving oral hypoglycemic drugs (odds ratio, OR= 0.34, 95% confidence interval, CI-=0.14 - 0.81, P=0.012) and patients with less than 5 years of diagnosis (OR= 0.53, 95% CI=0.30 – 0.95, P =0.034), were less likely to have poor glycemic control. There was no difference in glycemic control among patients by age, gender, BMI, type of diabetes, proteinuria, adherence, uncontrolled hypertension, presence of comorbidities and dyslipidemia, HbA1C, number of days of physical activities, level of education, employment or number of visits (Table 2).
Pathologic proteinuria (OR= 2.20, 95% CI=1.04 - 4.70, P =0.04) and patients receiving oral hypoglycemic drugs and insulin (OR= 2.58, 95% CI: 1.06 - 6.31, P =0.03) had a positive and significant effect on the outcome (Table 3). These patients were twice as likely to have poor glycemic control.
DISCUSSION
Diabetes is a chronic disease that significantly affects the quality of life of patients.15 The morbidity and mortality linked to this disease and the possible long-term complications represent a heavy burden for the family and society.16 The main objective of the management of a diabetic patient is to achieve optimal control of glycemia, which would reduce the occurrence of complications. Identifying and correcting factors linked to poor glycemic control is a big challenge, especially in a low-income country.
Though this study is cross-sectional, we found that 67.2% of the patients did not achieve their glycemic goal. The studies in our review are almost unanimous in noting that most patients have poor glycemic control, with extremes ranging from 61.9%17 to 91.8%18 in countries with a socioeconomic background like Haiti. In the USA, this rate of poor glycemic control is about 12.9%.19 Different baseline knowledge of the disease between these two populations, lack of consistent recommendations for optimizing glycemic control, presence of health insurance, and uneven health insurance coverage and access to primary care are other factors that influence glycemic control.20,21
Women are more likely to consult than men, due to better health seeking behaviors according to a CDC report.22 The strong female predominance of our population, 84.96%, can undoubtedly be explained culturally by the image of a stoic husband, who is a hard worker and provider of the family, making the diagnosis of certain chronic diseases rarer among them. The studies are not unanimous on this subject, with the prevalence varying according to the study. Conversely, men tend to be more insulin resistant due to a greater distribution of visceral and hepatic fat.22,23 A study has shown that women in charge of the household neglect their health and have worse glycemic control as a result.24 Several studies have shown that glycemic control becomes increasingly difficult as people age.16,25,26 However, this difference was not identified in our study.
In our study, patients receiving oral hypoglycemic drugs and insulin are 2.5 times likelier to have poor glycemic control, a finding similar to other studies included our review.22,27 Diabetes is a progressive disease, that is increasingly becoming challenging to manage pharmacologically if patients need additional drugs to optimize their treatment. Therefore, ensuring good patient education and finding strategies to reinforce patient compliance instead of adding drugs or maximizing doses have been proposed.28 Following the same line of thought, a long duration of diagnosis is associated with bad glycemic control because of the progressive exhaustion of the beta cells of the pancreas evolving towards an insulinopenia and making the dietary changes and the oral drugs less effective.29 We also noticed in our study that patients with less than 5 years of diagnosis had better glycemic control than those with a much longer duration of diagnosis.
A low level of education, was linked to poor knowledge of the disease, risky health behaviors and irregular monitoring. In contrast, a higher level of education is associated with the more active participation of patients in their care.23,30 Employment status did not show a statistically significant association in our study. Although one study showed that being employed meant that patients had less time to fully devote themselves to controlling their disease.25
Only 43% of our patients exceeded more than 10 visits over the year. This suggests that patients need to be encouraged to attend scheduled visits. An effective approach to improve attendance is by reinforcing education on the benefits of participating in regular physical activity which is associated with better glycemic control.28,31 Even though the strength of the association between physical and glycemic control is still debated, certain studies mentioned lack of time granted to physical activity, appropriate space or even the weather as the probable cause.32,33 It is an aspect that should not be overlooked in the counseling given to the patients.
Patients with hypertriglyceridemia and elevated LDL showed a statistically significant association with poor glycemic control,15,34,35 probably due to the prolonged entry of fatty acids into beta cells causing lipotoxicity, which in itself is responsible for the relative insulin deficiency.36 However, this was not replicated in our study, although 42% of patients had dyslipidemia. Nevertheless, since we did not ascertain the use of other medications from patients, it is possible that the use of lipid-lowering drugs played a role.
Hypertension, being obese or overweight were the main comorbidities identified in our study. We found a link between poor blood pressure control, hyperglycemia,16 and obesity.37,38 Although this has not been proven in our study, we want to emphasize that good control of glycemia also requires optimal treatment of blood pressure. Proteinuria is an important presumptive element of end-stage chronic kidney disease and a modifiable risk factor for cardiovascular mortality.39,40 Hypertension, duration of diabetes and obesity are risk factors for pathological proteinuria.41 The presence of pathological proteinuria is linked to poor glycemic control in our study, we should therefore emphasize a holistic approach in the intervention strategy and the management of diabetic patients among the study population. We should seek to understand the barriers against compliance, dietary habits, management of diabetes and comorbidities.
Non adherence to diabetic medications and using more than one oral hypoglycemic drug were statistically linked to poor glycemic control in this study in Tanzania.33 Poor glycemic control reached 83% in this study in Indonesia and was linked to medical adherence.32 Based on HbA1c values, 91.8% of diabetic patients had poor glycemic control, which was statistically linked to obesity, dyslipidemia and BMI in this study published in India.18 Nearly two-thirds of patients had poorly controlled diabetes in this study in Ethiopia, probably due to age, exercise, level of education, duration of treatment and smoking.25 Another study in the same country revealed 70% of poor glycemic control among diabetic patients, statistically linked to poor medication adherence and taking a combination of insulin and oral medication.27 In Brazil, over 60% in the study population had HbA1c levels >7%, which was associated with insulin use and less frequent follow-ups.30 Good medical adherence reached nearly 51% in our study. Though it didn’t reach statistical significance, counselling on medical adherence is a cornerstone in ambulatory patient care.
Our study has limitations. Important elements contributing to good glycemic control have not been assessed: diet and lifestyle habits, other medications that could alter glycemic metabolism, the presence of infections, types and numbers of oral hypoglycemic drugs used, and the level of understanding of the disease. There is selection bias based on the solitary measurement of glycemia to assess good control of chronic disease and information bias during the interviews. Causality cannot be inferred due to the cross-sectional nature of our study.
CONCLUSIONS
Considering the complex factors preventing optimal glycemic control in diabetics, their identification and a subsequent strategic approach would be an important step towards reducing acute and chronic complications, rational use of services and less cost. Findings from our study suggest that receiving oral hypoglycemic drugs, insulin and the presence of pathologic proteinuria are factors linked to poor glycemic control. Strengthening the education of the patients before optimizing pharmacological treatment would lead to better control, hence preventing renal complications. A larger study considering other potential barriers would be necessary.
Acknowledgements
First, we want to thank God for his infinite grace, making this work possible and for having placed on our path these people, whose contributions are invaluable:
-
Dr Mary Clisbee, for her critical review of this article
-
Noël Roudelie, Louis Sionise and Camilus Guerline, in patient recruitment and coding
-
Residents working at the clinic during the study period: Dr. Léandre Frickson, Dr. Damas Gasner, Dr. Gérard Emmanuella, Dr. Thellus Dellunesa, Dr. Jean Virline, Dr. Jean-Bart Fara in the interviewing of the patients
-
Interns and residents in social work in clinical rotation at the clinic during the study.
-
The MMAS-8 Scale, content, name, and trademarks are protected by US copyright and trademark laws. Permission for use of the scale and its coding is required. A license agreement is available from MMAR, LLC., www.moriskyscale.com
Ethics statement
The study was approved by the Zanmi Lasante ethics committee (ZL IRB) (Application number: ZLIRB03212022) on March 22, 2022. An informed consent form, written in Haitian Creole, was signed by each patient agreeing to participate. This form contains the relevant information of the study and ensures the anonymity of the data collection form. A coding system made it possible to differentiate each collection form.
Data availability
Available upon reasonable request to the corresponding author
Funding
This research received no external funding.
Authorship contributions
Principal investigator: Dr. Ludentz Dorcélus (conception, design, data interpretation, writing and revision of the manuscript). Co-investigator #1: Dr. Alexandre Emmanuel Rotchild (conception, design, data interpretation, writing and revision of the manuscript). Co-investigator #2: Dr. Villemenay Charnee Magalie (conception, design, data interpretation, writing and revision of the manuscript). Co-investigator #3: Mr. Benjaminel Scaide (data analysis and interpretation, revision of the manuscript). Co-investigator #4: Dr. Eddie Charles (writing and revision of the manuscript)
Disclosure of interest
The authors completed the ICMJE Disclosure of Interest Form (available upon request from the corresponding author) and disclose no relevant interests.
Correspondence to:
Ludentz Dorcélus
Zanmi Lasante
Rue Savannah, Saint-Marc
Haïti
[email protected]