Universal access to qualified, skilled, motivated and equitably distributed health workforce is pertinent for the delivery of integrated people-centred health services needed for achieving national health sector goals and sustainable development goals.1–3 However, there remains a shortage of health workers which is projected at 10 million by 2030,4 which is more prominent in Africa5 and rural and remote areas.6 Health worker shortages are limiting the functionality of the health systems, and the achievement of set goals at global, national and sub-national levels.6 Several factors have been suggested to result in the shortage of health workers, including low production of health workers, weak human resources for health (HRH) planning and management practices, and emigration.2 Furthermore, these shortages have been attributed to health workers’ choices of not taking up postings or staying in the locations they are posted. Some suggested reasons are preferences for opportunities that will lead to improved professional outcomes through opportunities for furthering education, being prioritized for in-service training, and to enhance clinical skills.7 Understanding the contextual issues driving the choice of workplace location by health workers is pertinent in designing and implementing tailored interventions for attracting and retaining health workers, thereby ensuring the equitable distribution of health workers.
Nigeria is striving to achieve universal health coverage (UHC) through primary healthcare revitalization by ensuring equitable access to quality health care services.8,9 This can only be achieved by improving access to and equitable distribution of qualified, skilled and motivated health workers. However, evidence on factors influencing the choice of workplace location, which is important in formulating interventions (including incentives) for ensuring attraction and retention of health workers in Nigeria is limited.10–13 This highlights the need for further evidence on the contextual meanings placed on workplace location choices based on health workers’ experiences which is pertinent for developing evidence-based policies and incentives for strengthening Nigeria’s health system.8,9,14,15 This study, therefore, adds to available evidence from the view of primary healthcare workers who work at the entry point into Nigeria’s health system. This study sought to understand the factors influencing primary healthcare workers’ choice of workplace locations.
METHODS
Study design and settings
This study applied a qualitative research design16 with the consolidated criteria for reporting qualitative research (COREQ) used to guide the reporting (see Online Supplementary Document).17
This study was conducted in Bauchi and Cross River States in Nigeria. Bauchi State is located in the North-East region of Nigeria consisting of 20 local government areas (LGA). It has a high burden of diseases and a projected population of over 6 million.18 Cross River State is located in the South-South region, and has 20 LGAs and a projected population of more than 4 million.18
Recruitment
A purposive sampling method was employed to recruit respondents in Bauchi and Cross River States of Nigeria. Eligibility for participation was dependent on being a nurse, midwife or community health practitioner (community health officer (CHO), community health extension worker (CHEW) or junior community health extension worker (JCHEW)) providing health services at primary health care centres in any of the local government areas. The tentative respondents were selected from a list of potential interviewees drawn by the gatekeepers – leadership of the primary health care development agencies in both States. Forty-one respondents (16 from Bauchi State (BAU) and 25 from Cross River State (CRS)) were approached physically in their workplaces using a participant information sheet and requested to participate in the study. All approached key informants agreed to participate in the study and were interviewed.
Data collection
The investigators developed a semi-structured interview guide following a review of the literature. Semi-structured interviews were conducted by the two investigators (SCO and CN) between August and October 2018 to ensure consistency in questioning and immersion in the data collection process. The investigators are experienced and trained qualitative researchers. The interviews aimed to understand the factors influencing health workers’ choice of workplace locations focusing on factors that may either attract or retain health workers in postings. The guide used for the interview elicited responses on the important issues that health workers consider when thinking of a work location. Following initial questions, the interviewers asked probing questions to gain further insights into how each mentioned factor influenced their choices. By applying a semi-structured qualitative approach, respondents described their perspectives within 40 to 60 minutes until saturation was achieved19 with no new themes or perspectives evolving. All interviews were conducted in English and recorded using a voice recorder with notes also taken.
Data analysis
The interviews were transcribed verbatim for analysis with respondents anonymised. Analysis of transcribed data was managed using the NVivo software®. Two investigators (SCO and CN) applied the principles of a phenomenological analysis process by gaining a holistic impression of the information by reading all transcripts, categorising pieces of meanings (themes) and coding them, condensing the meanings of the themes; and synthesizing the descriptions.20,21 SCO and CN analysed the interview transcripts independently and reached a consensus on the final themes and descriptions.
RESULTS
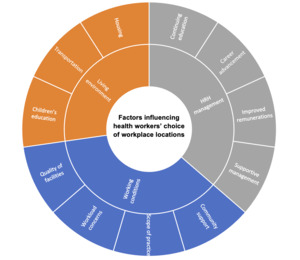
The analysis identified three major themes that were apparent as factors influencing health workers’ choice of workplace locations. The themes included: (i) working conditions, (ii) living environment, and (iii) HRH management (see Figure 1).
Working conditions
Quality of facilities
The quality of facilities, in relation to the availability of needed medical equipment and spaces, was important to both the health service provider and the patients that visit, and this influences the choice of work locations for health workers.
The health workers reported that based on their experience, health facilities in rural areas often do not have needed medical equipment for quality service delivery when compared to those in urban areas.
“From what I saw during my postings in the rural area, the provision of equipment is less in the rural area than what we have in the urban area.” - CRS 1, CHEW
According to the respondents, health workers are reluctant to accept postings to health facilities that are not well equipped. This is because the standard determines if patients will attend the facility and they can deliver quality services without being faced with avoidable risks of infection.
“The standard of the health facility is important to both the health worker and to the clients coming in. If the standard of the facility is not up to the expectation of clients, they will not come. For the health worker, trying to improvise puts you at risk. So, I will not go to a facility that does not have equipment.” - BAU 11, CHEW
Respondents indicated that the facilities in urban areas often have appropriate medical equipment compared to the rural ones and this ensures health worker safety and proper service delivery. In contrast, the lack of relevant medical equipment, which is prominent in rural areas, results in health workers improvising whilst delivering health services.
“A health worker will be exposed to more hazards in a rural area than in the urban area because while working there, those in the rural area improvise a lot more than those in the urban area, because, at times, the needed facilities or equipment will not be there.” - CRS 15, CHO
The health facilities in the urban areas were reported to receive more attention from the government and partners. This ensures that they have medical supplies and equipment, and the designated and apposite spaces for delivery of health services. In contrast, the health facilities in the rural areas were often not in line with the government infrastructure standards resulting in the allocated spaces for service delivery not being suitable.
"What differentiates the facilities in the rural area and that of the urban area is the government pay more attention to the ones in the urban area, they get more equipment and space to provide health services. In the rural ones, the facilities are small with different services provided in the same space." - BAU 9, CHEW
To gain needed experience on how to deliver quality health services, health workers in rural areas often leave rural postings for urban ones and often strive not to return to rural postings. This is continually reducing the availability of skilled health workers needed to deliver health services to the rural populace.
“The reason a health worker would want to move out from the rural community to the urban one is to have more experience because in the rural area you don’t have the equipment to deliver good health services.” - BAU 3, CHO.
Workload concerns
Most respondents indicated that the workload of health workers is higher in rural areas when compared to the urban areas and this also influences the choice of work location for health workers.
“The workload is very high in the rural area because we are very few. In some facilities, only one person provides services 24 hours a day.” - BAU 8, CHEW
The health workers further highlighted that the high workload is mainly due to inadequate staffing to address the patient’s needs. This often results in health workers having to take most of or all the shifts in a bid to ensure that health services are provided to clients.
“Actually, in the rural area, the working population or the workforce is less as compared to the urban area. If you go to some facilities, you have just two health staff and they are expected to run morning, afternoon and night shifts.” - CRS 22, Nurse
Inadequate staffing was also mentioned as limiting health workers in rural areas from taking time off for leave, training or further studies. This was indicated to be due to the absence of another health worker to provide needed cover. According to the respondents, the health workers in the urban areas have more opportunities to enhance their education and skills due to the availability of other health workers to provide cover in health service delivery.
“Those in the urban have more opportunities because if you go to the urban area, they have many hands to do the work and if you go to upgrade your capacity, it would be easier for you. You won’t be tied down because someone is there to replace you but if you go to a rural area when you are two, you will find it difficult to leave the facility.” - CRS 12, CHO
Respondents further highlighted that due to the availability of various categories of health workers in the health facilities in urban areas, the workload is reduced.
“If you go to the rural area, sometimes there is no manpower there. So, you discover that in the rural areas, the people there are suffering. But here in the urban area, they have lots of manpower for different roles.” - BAU 7, CHO
Scope of practice
The scope of services provided in settings also influences health workers’ choice of workplace location. The respondents stated that the scope of services they provide is guided by pre-service education and in-service training, scheme of delegation and directives by supervisors or senior colleagues.
“We work based on the scheme of delegation, our training and what we are told.” - BAU 7, CHO
In rural areas, the scope of the activities conducted by cadres is often dependent on their numbers as well as the availability of other cadres. The scope of services provided in rural areas is broader due to the absence of other cadres needed to deliver health services and experienced colleagues who can perform services requiring experience and critical care. This encourages some health workers in need of some autonomy to choose to work in rural areas as against urban areas where the scope is reported to be confined to roles based on pre-service training.
“Some health workers prefer to work in rural areas so they can deliver services that other health workers are supposed to, mainly because it gives them satisfaction to provide additional services that they are not primarily supposed to.” - CRS 22, Nurse
On the other hand, the health workers also indicated that some health workers also prefer urban facilities to allow them to provide more specialized services or learn specialized skills and experience.
“People move to the urban area to gain more experience from older colleagues and other health workers.” - BAU 6, CHEW
Community support
Respondents stated that health workers often obtain information on whether the community members seek services from a health facility or rely on services provided by other sources including faith-based and traditional attendants. Additionally, they also learn of the prevailing cultural practices and norms that guide health service-seeking behaviour. Knowledge of these informs the choice of workplace location.
“There are some villages where people don’t like going to their health facilities due to one belief or the other.” - BAU 11, CHEW
The prevailing community acceptance practices were also indicated as an important aspect that health workers consider as they do not often take up or stay in postings where acceptance levels are poor as these impacts negatively on health service provision and utilization.
Also, the respondents indicated that the community’s level of involvement in the health facility management process through the community development committees was important to them. According to the health workers, the level of participation indicates the extent of support they would receive from community members whilst providing health services.
“I will also like to know if the community are participating in the facility management.” - CRS 20, CHEW
The health workers stated that community participation is usually higher in rural areas. Also, where health workers are accepted, the community members ensure that they are comfortable and have the needed conducive environment to deliver health services.
“Community support in the rural areas is higher and they always tend to see how the health workers will be comfortable. When the health workers have any problem, the community people come together and agree on how to help these health workers.” - BAU 8, CHEW.
Living environment
Housing
All respondents reflected that the availability of housing (or “accommodation” as often called in the study setting) is critical in workplace location choice in both rural and urban areas. The presence and availability of accommodation within the health facility premises (often referred to as “quarters”) is a predominant factor. According to the respondents, its absence results in health workers having to convert some space within the health facility into a residence.
“Accommodation is one of the problems especially if the person is posted to a facility where there are no quarters or if the quarters are filled up. The person may end up sleeping in the facility.” - CRS 21, CHO
Many suggested that the availability of good quality housing in rural facilities attracts health workers because of the associated cost savings in paying to rent quality accommodation in urban areas which is expensive.
“I believe if housing is provided, definitely, health workers would like to stay in a rural area. Accommodations in urban areas are quite expensive.” - BAU 6, CHEW
The respondents also stressed the importance of being paid a housing allowance which is done to enable health workers to rent an accommodation. In practice, however, the payment of this allowance is not consistent, resulting in health workers not getting quality residences.
Many stressed the need for government to target health workers in rural areas for payment of a housing allowance to enhance their ability to rent quality houses. According to them, this should be implemented for all health workers in rural areas as the quarters are often not of sufficient quality for the health workers and their families.
Transportation
The respondents suggested that some health workers prefer commuting to work, thus making the availability of suitable transportation mechanisms an important factor. The reasons suggested to result in the aforementioned include the urge to stay with family, the absence of housing within facilities, and to safeguard the health workers’ mental health.
"We usually check the time it will take us to go to work and return home to our families, because we need to also dedicate time to attend to our family needs." - CRS 7, CHO
Additionally, how safe the transportation routes to health facilities are was reported by many respondents as vital in accepting postings and being at work to deliver health services to the populace. This was highlighted to also be a contributory factor to the absenteeism of health workers who do not reside within health facilities.
“I will not accept a posting to a facility where the roads are not safe for me to travel to work and return home when I finish my shifts.” - CRS 14, CHEW
Children’s education
The importance of the health workers’ children accessing quality education was stressed by the married women respondents. They highlighted that the quality of public schools in rural areas is inferior and this informs their preference for private schools which are often expensive.
“The rural areas usually do not have affordable good schools, and this is why most of us do not want to go and work there.” - CRS 20, CHEW
Furthermore, they indicated that private schools are often not also available in most rural areas and this influences their choice of wanting to take up and stay in rural postings.
"It is important to me that my children attend good schools and so if they are not available, I will not want to stay in the facility." - BAU 8, CHEW
HRH management
Supportive management
The respondents reported a general dissatisfaction with the lack of supportive management of policymakers and health managers. They highlighted that the effort being put into delivering health services within the current context of the health system was not acknowledged. The importance of appreciation of the health workers’ contributions by superiors was stressed to be important to health workers.
"The management does not understand and appreciate what we pass through to provide health services. When they appreciate it formally or informally, it motivates us." - CRS 9, Midwife
Similarly, respondents indicated that the work relationships with supervisors and superiors are often not cordial, and this also affects the choice of work location. They highlighted the importance of a friendly work environment in motivating health workers to take up and stay in work locations.
“Then in the relationship between bosses and subordinates, there are some subordinates who like to work in an atmosphere where the supervision is friendly.” - BAU 13, CHO
They also indicated the importance of a supportive management process, highlighting that the health workers are inclined to take up and stay in postings where they actively participate in co-creation, decision making and programme implementation.
“Recognition, allowing people to suggest and giving them opportunities to be themselves and be contributing to whatever programmes are being implemented gives people satisfaction.” - CRS 18, CHEW
In highlighting the resultant effects of a weak supportive mechanism on the health system performance, the current lack of quality service delivery data was stated.
"The authority doesn’t carry out supervision that was why there is no accurate health service data." - BAU 15, Nurse
Additionally, the respondents attributed the reported sub-optimal quality of health service delivery in rural areas to the weak supportive systems.
“The supervisors do not regularly go and check the activities of the workers in rural areas, so the quality of health care provision is better in the urban area.” - BAU 12, Midwife
Improved remunerations
All respondents stated that salaries were an important factor for health workers and efforts should be made to pay health workers’ salaries promptly as against the current practice whereby health workers are owed their pay for several months. They also highlighted the need for improved salaries to reduce the migration of health workers to other sectors and to other countries.
Also, an increase in the salary paid to the health workers posted to rural and remote areas, compared to those working in urban areas, was suggested as important in attracting and retaining them.
"The health workers in the rural areas should be paid more than those in the urban areas to motivate them to stay." - CRS 17, Nurse
"The health workers in the urban areas have access to many social facilities than the ones in the rural areas. So, it’s only appropriate that the ones in the rural areas should be paid more salary." - BAU 2, Nurse
Respondents also specified the need for additional monetary incentives, beyond basic salaries, to attract and retain health workers in rural and remote areas. They indicated that this is pertinent in ensuring that availability and access to qualified and skilled health workers needed for delivery of quality health services.
“There should be something extra that should entice people to go to rural areas. You see those people hanging around in urban areas, if there is any rural package, you will see them running back to the rural areas.” - BAU 9, CHEW
Career advancement
According to the respondents, the prospects of career advancement play a critical role in the choice of workplace location. One important aspect mentioned by the respondents was the importance of promotions being implemented promptly.
"The authorities should be promoting us when due. They usually delay promotion exams and implementation of promotion." - CRS 18, CHEW
Also, the need to make health workers’ service duration in the rural areas count during promotion exercises was suggested to be made a strong consideration. Specifically, the health workers suggested that the number of years needed to participate in promotion exercises be reduced for those serving in rural and remote postings. This, they suggested, would further enhance the attraction and retention of health workers in these areas.
"If they could reduce the number of years for promotion for those in rural areas, it will encourage them to stay there and also attract other health workers." - CRS 4, Midwife
Respondents also stated that to ensure equitable management of health workers, the government should put mechanisms in place to ensure periodic rotation for all health workers to rural and urban areas, thereby making rural service compulsory for all health workers.
Continuing education
Gaining further knowledge through in-service training and post-graduate education was suggested by all respondents as pertinent to the delivery of quality health services. The respondents reported that workplace locations in urban areas are preferred as this avail an opportunity to undertake post-graduate education mainly due to proximity to training institutions, and this also increases prospects for growth within the public service.
"Those in urban areas have a better opportunity to study more than us in the rural areas and this makes them get promoted before those in rural areas." BAU 12, Midwife
Another enabling factor mentioned was the presence of other health workers to provide cover during absences in the urban areas which is not the case in facilities located in rural areas.
"Now if a health worker in a rural area wants to go to school, there is going to be just one staff left to run the shifts. So that alone will be a barrier. But if you go to the urban area where you have up to five staff in some facilities. If one wants to go to school, the other ones can adjust." CRS 14, CHEW
Respondents stated that the prospect of an opportunity to participate in in-service trainings sponsored by the government or partners is limited for health workers in rural settings with those in urban areas being given preference.
"Those in the urban area benefit more from attending trainings than those in the rural area. Most times they forget the health workers in the rural areas and we don’t benefit from trainings." CRS 22, Nurse
DISCUSSION
We aimed to understand the factors influencing the choice of work locations amongst primary healthcare workers in Nigeria and the underlying drivers of the choice processes. We applied a qualitative approach because it allowed for the gaining of rich descriptions of the factors which are important in developing tailored policies and strategies to improve the equitable distribution of health workers. The respondents comprised of the highest proportion of cadres providing health services at the primary level of care in Nigeria (nurses, midwives and community health practitioners) to gain a diverse view pertinent to HRH planning and management.
Our study found that the working conditions influences the choice of work location to a great instance. Quality of facilities was reported as a key factor that influences health workers’ choices. With facilities in urban areas having better medical equipment and infrastructure in most parts of Nigeria,22 this plays a key role in the skew in health worker distribution in favour of the facilities in urban areas. Beyond medical equipment and apposite spaces being pertinent for quality service delivery, another perspective raised was their importance in encouraging clients to visit health facilities to seek health services and ensuring patient and health worker safety. These are key and have been highlighted as vital for quality service delivery23 as their absence deters the use of health services by clients.24,25 An important perspective gained from this study is the internal migration of health workers from health facilities in rural areas to urban ones to gain skills and experience, with a reduced likelihood of returning to the rural area. This further highlights the need for facility standards to be set and adhered to across rural and urban areas. This will contribute in ensuring that needed experience can be obtained in facilities in urban and rural areas. Additionally, compulsory posting of health workers to health facilities in rural and urban areas whilst in service can be institutionalized.
The varied staffing levels in rural and urban areas were also suggested to be a factor influencing the choice of work location in relation to concerns about the workload to be faced and the scope of tasks that can be performed. The finding that workloads are often not matched to staffing levels has been reported within the study setting26–30 and is consistent with the literature.31,32 With the impact of high workloads and the broader scope of practice felt more in rural areas, with some health workers providing services all through the day, and not taking time off for leaves and other career enhancement activities, policymakers should ensure mechanisms for apposite staffing are instituted. The conduct of periodic staffing needs assessments and the use of the evidence for redistribution of health workers will play a huge role in ensuring equitable distribution of workloads to existing health workers. Equally, ensuring the availability of all pertinent staff categories would also ensure professionalism, apposite quality service delivery and reduced workloads on available health workers. In instances where health workers are expected to deliver health services beyond their pre-service training, measures should be put in place to ensure they are trained and mentored to ensure quality health service provision.
Cultural practices and norms were reported by respondents as affecting health-seeking behaviour and services utilization as has been evidenced in other countries.33 Related to this are the community participation and acceptance practices which health workers consider. Strong community participation is critical for the delivery of integrated people-centred health services34 and resultant improved population health outcomes.35 Community acceptance is also important as reported by the respondents because it reassures health workers that they will be supported by the community. Our findings indicate the need for policymakers and health planners to strengthen community involvement in health sector priority setting and implementation as it contributes to the achievement of health sector goals and health worker attraction and retention. This can be achieved by ensuring a bottom-to-top planning of health strategies and the involvement of community representatives in national level planning actions.
We found that the choice of workplace locations is influenced by the living environment obtainable by health workers. Specifically, the availability of quality housing or an allowance that is sufficient to pay for a quality accommodation, availability of transport facilities that are not far from places of current residence and are secure for frequent travels, and quality schools for children’s schooling were suggested as important factors. This finding aligns with the literature on the importance of social amenities in ensuring attraction and retention of health workers.13,36,37 Whilst the provision of social amenities is beyond the control of the health sector, our finding highlights the importance of the health sector to factor in housing in its health infrastructure plans or housing allowances in lieu. They should also advocate for transport routes through health facilities to ease transport needs for health workers and clients, and the inclusion of building quality schools in national and sub-national development plans.
The respondents mentioned that the implementation of effective HRH management practices, which often vary in rural and urban areas, are critical factors that influence the choice of workplace locations amongst health workers. Weak supportive management was specified with emphasis made on leadership not appreciating work being done within prevailing circumstances, work environment not being cordial, and non-involvement of everyone in co-creation, decision making and programme implementation. Health workers also stated that salaries should be paid along with increased packages for health workers posted to rural and remote areas. Similarly, the importance of prompt implementation of promotion was indicated with suggestions for special considerations for health workers in rural areas. Of keen interest to health workers was fair treatment with mandatory rotation to rural and urban areas for all health workers, and access to further education opportunities. HRH management processes have been widely reported to be weak at various levels due to various reasons. All these are negatively impacting on health worker attraction, motivation and retention.38–41 There is a need to streamline HRH management processes by improving the capacity of HRH managers at various levels in leadership and management, and ensuring that equal opportunity and fair treatment principles ensue.
Our study has some limitations. The study was conducted in two States in Nigeria which suggests that the extent to which the findings can be generalized to Nigeria is limited. However, the States are located in the northern and southern parts of the country and we feel our findings highlight pertinent factors influencing the choice of workplace location taking into account the dynamics in these two geographical locations. Still, further research in other States is recommended. Secondly, we did not collect information on the demographic characteristics of respondents and use this to compare views based on age, gender, length inservice, and marital status. This was done deliberately as we intended to gain a general understanding. We recommend further research considering this to determine if views vary based on the aforementioned dynamics.
CONCLUSIONS
Our study highlights the importance of work location to health workers. Furthermore, it indicates the need for policymakers and health planners, at all levels of the health system, to gain and apply contextual evidence on factors influencing health workers’ choice of workplace locations in health and HRH planning and management. This is pertinent in designing and implementing tailored interventions for attracting and retaining health workers, thereby ensuring the equitable distribution of health workers.
Acknowledgements
The authors wish to acknowledge the support of the Bauchi and Cross River State Ministries of Health, and State Primary Health Care Development Agencies.
Ethics statement
Ethical approvals were obtained from the National Health Research Ethics Committee of the Federal Ministry of Health as well as the State Institutional Review Boards. Written informed consent was obtained from all respondents prior to taking part in the research.
Data availability
Data are available upon reasonable request.
Funding
This work was funded by the Global Affairs Canada under the Enhancing the Ability of Frontline Health Workers to Improve Health in Nigeria Project - A-035024/l. The APC was funded by the authors.
Authorship contributions
SCO and CN drafted the initial manuscript. SCO JAA, AA and MKO conceived the study. SCO designed the protocol. SCO and CN designed the tools and conducted data collection and analysis. All authors read and approved the final version of the manuscript. SCO acts as the guarantor.
Disclosure of interest
The authors completed the ICMJE Disclosure of Interest Form (available upon request from the corresponding author) and disclose no relevant interests.
Additional material
The consolidated criteria for reporting qualitative research (COREQ) checklist used to guide the reporting is included as Online Supplementary Document.
Correspondence to:
Sunny C Okoroafor
Universal Health Coverage - Life Course Cluster,
World Health Organization Regional Office for Africa,
Brazzaville, Congo.
[email protected]; [email protected]