With the 2019 projected population of over 200 million,1 Nigeria is the most populous country in Africa and has the largest concentration of health workforce on the continent. Over the past two decades, Nigeria has made concerted efforts to reduce child mortality through developing policies and implementing child survival strategies and interventions. One such action is the Integrated Maternal, Newborn and Child Health (MNCH) strategy in 2007 and its revision in 2013, with the goals of improving access to quality health services; strengthening the capacity of individuals, families and the community to take necessary MNCH actions at home; and recognising when to seek appropriate health care. The strategy also aimed to establish a financing mechanism that ensures adequate funding, affordability, equity, and efficient use of funds from various sources.2
While the 2018 Nigeria Demographic and Health Survey (NDHS) showed that the under-five mortality rate declined from 193 deaths to 132 deaths per 1,000 live births between 1990 and 2018 (a decline of 31.6%).3 Nigeria is the largest contributor to child deaths globally, recording about 900,000 deaths in a single year.4 The current effort at reducing the under-five mortality rate in Nigeria is significantly slower than what is needed to achieve the Sustainable Development Goals targets of reducing child mortality to 25 deaths per 1,000 live births and neonatal mortality to at least as low as 12 deaths per 1,000 live births by the year 2030.5 Reversing the current trend and moving Nigeria closer to the goals require urgent policy interventions based on an in-depth understanding of the contexts of child health care and paths to survival, particularly in those geopolitical zones where child health outcomes are most worrisome.
Studies have shown that child survival is intricately linked to socio-economic factors such as poverty and behavioural and cultural issues.6–10 Safe drinking water and good hygiene are less available in poor households, where people are also more likely to have difficulties accessing timely and quality healthcare and often cannot afford nutritious diets. Improving the social determinants of health by strengthening the capacities and awareness of individuals, families, and communities is key to producing the desired health outcome in children.11 In most countries, including Nigeria, effective maternal and neonatal healthcare interventions are available; thus, the desired reductions in childhood mortality could be achieved by increasing their coverage.
The 2019 Verbal and Social Autopsy (VASA) survey provides updated information on Nigeria’s causes and social determinants of under-five deaths. The survey was conducted based on deaths identified in the 2018 NDHS. Compared to a prior Nigerian VASA study conducted in 2014 based on the NDHS 2013, the 2019 VASA allowed inclusion of more qualitative responses and a complementary qualitative study to help understand the social determinants of causes of death in under-five children.
This study presents the social autopsy component of the 2019 VASA with the overall objective of providing an in-depth understanding of typical household, community, and health system determinants of under-five mortality in Nigeria. This paper is intended to guide policy-makers to make evidence-based decisions and design programmes to improve under-five survival in Nigeria and other low- and middle-income countries.
METHODS
Study design and sample
This study was a cross-sectional, nationally representative survey of all 36 states of Nigeria and the Federal Capital Territory based on the 2018 NDHS. A multistage sampling procedure was employed to select 42,000 households sampled during the 2018 NDHS. Out of this number, 4,096 households were identified with a history of under-five deaths in 2013-2018. Of these, 3,993 gave consent during the NDHS for a follow-up study to provide information on the signs and symptoms of the fatal illnesses of the deceased children. Three thousand, two hundred and fifteen (3,215) households (81% in Nigeria’s northern three zones and 19% in the southern three zones) participated in the survey (Table 1). In some households, two or more under-five deaths were reported for the sampled period. However, due to the possibility of overlapping environmental and health system determinants of the causes of the deaths within the same household, as well as to reduce the burden of the interview for families, the most recent death was selected in households with more than one death for the study.
Study instrument
The 2019 VASA survey instrument was adapted from the 2016 WHO Global Standard Verbal Autopsy Questionnaire.12 The social autopsy topics not included in the WHO standard were supplemented with questions from the Nigerian 2014 VASA survey instrument13 adapted from the Child Health and Epidemiology Reference Group (CHERG) social autopsy questionnaire.14 The study instrument consisted of 14 modules grouped into three main sections, as presented in Table 2.
The study instrument was translated into the three major Nigerian languages: Yoruba, Igbo, and Hausa. The translated instruments were back-translated into English to preserve the validity and contents. The survey instrument and translated versions were programmed into the Census and Survey Processing System (CSPro) software application that enabled the interviewers to capture data directly into a netbook computer.
Recruitment and training of interviewers
A total of 53 field researchers and 15 supervisors were recruited for the study. These researchers and supervisors were experienced in quantitative data collection, familiar with the study setting, and fluent in English and at least one of the local languages of the area. They underwent 17 days of training on the conduct of verbal autopsy as well as three days of field practice. The training focused on data collection instruments, interview techniques, ethical principles, eligibility criteria, and computer-aided personal interview use to capture data.
Data collection and quality assurance
The data collection period ran from October to December 2019. The trained data collectors visited the selected households to interview the mother/caregiver of each deceased child selected for the study. Where the mother was not available or not involved in the care of the deceased during the fatal illness, another caregiver who stayed with the deceased during the fatal illness was interviewed. Informed consent was obtained from interviewees before administering the study instrument.
Data quality was ensured throughout the data collection process through CSPro automated check on the range of values, skipping to the appropriate question aligned with responses given, and consistency checks of the collected data. Also, the supervisors carried out field checks of tables generated by CSPro while the field editor downloaded interview data daily to check for completeness.
Analysis
The 2019 social autopsy section looked at demographic information on neonatal and 1-59 months child deaths from the 2018 NDHS weighted to represent the Nigerian population. A descriptive analysis of the data was carried out to describe the prevalence of key household, community, and health system indicators of preventive and curative care for neonates and children 1-59 months along the continuum of care and the pathway to survival model. All results in the findings section (except for the cost table) were weighted according to the Nigeria DHS 2018 survey cluster weights to represent the national population. This social autopsy study builds on the causes of death found in the verbal autopsy analysis, which is available in the study report15 and published elsewhere.16
Illness severity was assessed when the caretaker first noticed the child was ill and at subsequent points of care decisions for those who sought care from a formal provider. This was built from questions about the child’s feeding behaviour, activity level, and mental status, each divided into three levels (normal, somewhat affected, or severely affected). These were further aggregated into an overall score of normal/mild, moderate, or severe following the method of Koffi et al. as described in a previous paper.17 The three levels of severity were assigned values of 1, 2, and 3 to compare average severity scores at different stages of care.
Data analysis was carried out using the STATA version 16.1 statistical package. The outputs from the analysis were presented as charts and tables illustrating the various social determinants of deaths. The chi-square test statistic was used to test differences in the distribution of categorical variables, while the Wilcoxon rank-sum test was used to compare differences in continuous variables and the level of significance level was set with P<0.05.
Ethics approval
The study was approved by the National Health Research Ethics Committee of the Federal Ministry of Health in Nigeria and the Social Solutions International Inc. Institutional Review Board in Rockville, Maryland, USA. Informed consent was obtained from each respondent before recruitment into the study.
RESULTS
Table 3 compares the demographic characteristics of deaths in neonates and children aged 1-59 months from 2013 to 2018, the period of the 2018 DHS survey, versus live births in the same period. This allowed calculations of the neonatal mortality rate and 1-59 months child mortality rate (per 1,000 live births) for this period. Data were from the Nigeria DHS 2018 survey and were weighted.
Neonatal mortality rates varied from a low of 33/1000 to a high of 46/1000 based on the wealth index. The variation in 1-59 months child mortality rates was much larger, ranging from 22/1000 to 130/1000. Using the chi-square test, the indices of children with neonatal deaths were not significantly different from those who survived the neonatal period by mother’s education, household electricity, improved water, improved sanitation, and cooking fuel used. Rural areas had marginally higher neonatal deaths than urban areas (P=0.033), and male newborns had slightly higher deaths than females (P=0.044). Findings by zone (with the North West zone having the highest mortality and the South East and South South the lowest rates) by mother’s age (with higher neonatal deaths at both the highest and lowest ages), and by wealth quintiles (with lowest neonatal deaths in the two highest quintiles) were all strongly significant findings (P<0.001) but there was no situation where the highest row rate was double the lowest.
In contrast, while not significantly different for males and females (P=0.423), mortality in children aged 1-59 months was significantly different for all the other characteristics in the table (P<0.001). Characteristics with multiple levels, except for maternal age, showed a consistent change from top to bottom and the highest group often showed four- or five-times higher mortality rates than the lowest group.
Maternal complications, care seeking and mortality by age groups
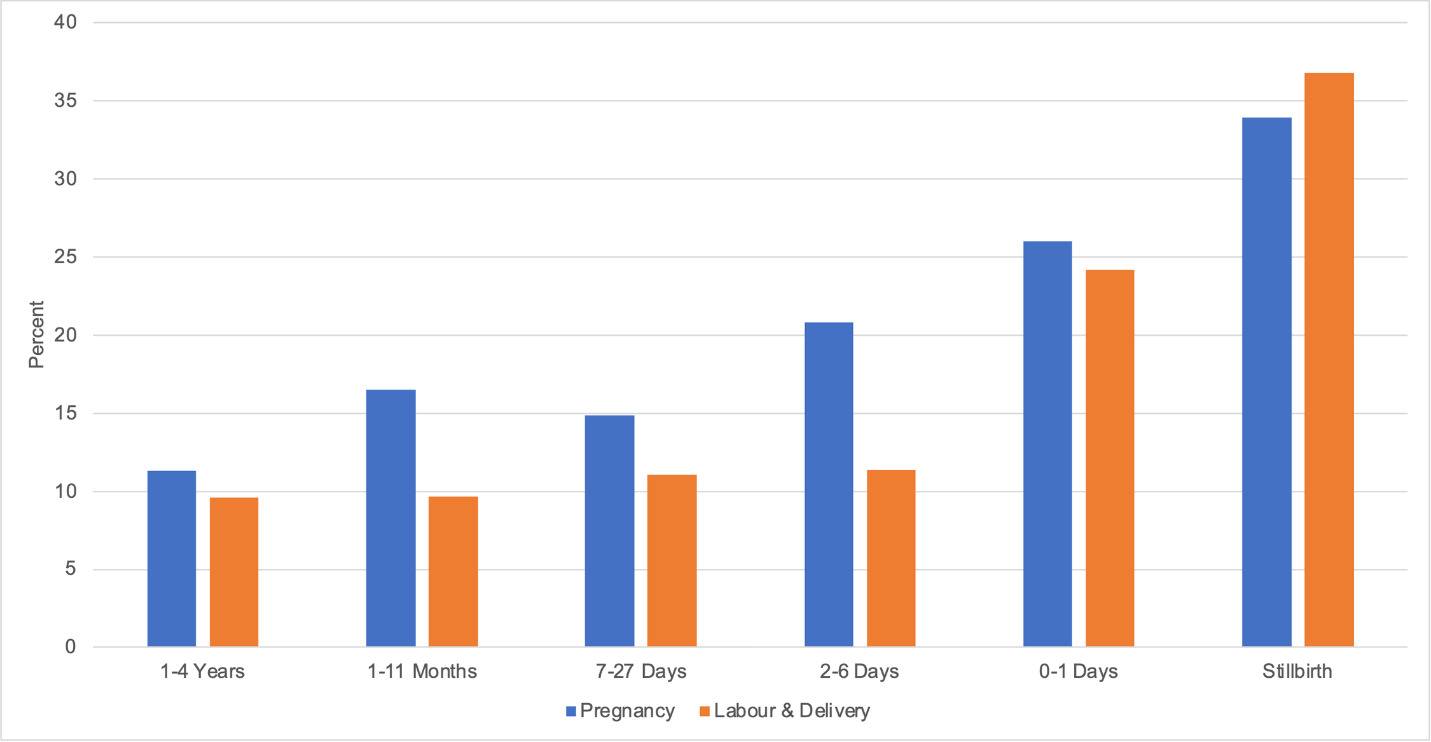
The VASA survey asked caretakers of all cases whether the mother had experienced complications during the last three months of pregnancy or during labour and delivery. Data on complications among women whose children did not die were not reported but comparing complication reports by the ages of death of the children provided a way to observe whether maternal complications were associated with early neonatal deaths (Figure 1). The rate of complications in pregnancy varied from 11-17% for deaths in the 1-59 months age group to about double this rate (26-34%) for stillbirths and deaths on the day of birth or day after (P<0.001). Reported labour and delivery complications were even more strongly associated with earlier deaths, ranging from a report of 10-11% in all groups after the first two days to two to four times as high (24-37%) in stillbirths and deaths in the first two days (P<0.001).
Women were also prompted about the presence or absence of a list of 13 specific pregnancy symptoms and 12 specific labour and delivery symptoms. The prompted list of symptoms increased overall reporting of pregnancy symptoms to 60-62% for stillbirths and deaths in the first two days compared to 37% for 1-11 months old deaths (P<0.001). Labour and delivery symptoms increased to 65-66% compared to 31%, respectively (P<0.001). These prompted figures suggest that over half of stillbirths and deaths on the day or day after birth were associated with symptoms in labour and delivery.
Among women who reported delivery in a health facility, complications in labour and delivery were significantly higher than those who delivered at home (26% compared to 11%, P<0.001). This pattern remained present regardless of the ages at death of the child (Figure 2).
Looking specifically at women with a stillbirth or death on the first or second day, 46% (198/428) of women with no complications delivered in facilities compared with 67% (115/171) (P<0.001) with complications. Assuming that complications were independent of the originally planned delivery place, it suggested a shift of 18% of women with complications related to deliveries to facility birth. However, most women with complications would not have shifted to a facility and still delivered at home.
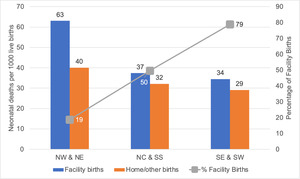
The higher rates of complications in facility deliveries corresponded to an observed higher rate of neonatal deaths in facility births in Nigeria (Figure 3). Birth and death data were taken from the 2018 DHS and divided into three groups according to overall facility birth rates. These were the North West and North East zones (with a 19% facility delivery rate), the North Central and South South zones (50% facility delivery rate), and the South East and South West zones (79% facility delivery rate). The neonatal mortality rate among facility births was significantly higher than for home births in the North West and North East zone groups (63/1000 live births compared with 40/1000, P<0.001) and North Central and South South zones (37/1000 compared with 32/1000, P=0.05), while there was no difference between facility and home births in the South East and South West zones (34/1000 compared with 29/1000, P=0.900).
Preventive and newborn routine services
Figure 4 shows many routine care and preventive services for neonates and children aged 1-59 months. Coverage for most interventions was relatively high (70-89%), but three aspects of essential newborn care—the rate at which newborns were placed on the chest/skin-to-skin contact, delayed bathing for at least 24 hours, and breastfeeding within one hour were all low (8-25%).
Nutrition
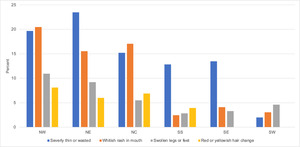
Malnutrition was not a common direct cause of death by either the physician-coded or expert algorithm methods (2-3% of 1-59 months deaths). This was because it was treated mostly as an underlying cause. However, rates were much higher when looking at specific questions related to malnutrition (Figure 5). For the four questions in the figure, overall rates were 7-19% of all deaths. In addition, all three signs of malnutrition (severely thin P<0.001, swollen legs P=0.006, and change in hair colour P=0.006) were much more common for deaths in the northern zones where the highest child mortality rates were found in the NDHS 2018.
Pathways of care
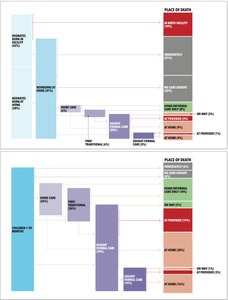
The responses to the series of questions asked for neonatal and child deaths regarding the sequence of actions from when an illness was first noticed until death are summarised in Figure 6. One of the most noticeable features of the neonatal compared with the child pathways is that among neonates, most deaths occurred either in the facility of birth before discharge or at home without any care. 72% of neonatal deaths had already occurred when care was sought in the home. In contrast, 88% of children aged 1-59 months in households sought or received some care for the final illness. For both groups, the proportion who died at a formal health provider, whether the initial or last, was smaller than the proportion who left the provider and died at home.
Death among births in health facilities
Among the 773 neonatal deaths analysed, 321 (42%) were born in health facilities. Of these, 148 (46%) died before they left the facility, making up 19% of all neonatal deaths; 89% of these deaths in the birth facility occurred on the day of or day after birth with intrapartum deaths (57% by expert algorithm analysis) as the major cause. Among the 173 newborns discharged from the birth facilities, 39 (23%) were reported to have been already sick. Over half of these went for additional formal care.
No care seeking for neonatal illness at home
Excluding newborns who died in birth facilities, there were 625 neonatal deaths and 2,152 child deaths in 1-59 months. Among the neonates who died at home, 237/625 (38%) were reported to have “died immediately” and 171/625 (27%) “did not receive or seek care”. These made up the largest proportion (53%) of all neonatal deaths in the study. Among the 1-59 months children, 134 (6%) were reported to have “died immediately”, and for another 132 (6%), no care was sought or received, making up 12% of deaths in this age category.
Among immediate deaths in neonates, the most common diagnoses (by physician coding) were “intrapartum” and “unspecified”, and for children 1-59 months, “sudden death” and “injury”. The survey’s definition of “died immediately” was limited to deaths within 24 hours of the child falling ill; however, the illness duration was two days or more for about 10-20% of cases. Looking at text comments, it was clear that some respondents interpreted “immediate” to mean that the child died “suddenly” or “unexpectedly” after what they thought was a mild illness rather than “immediately”.
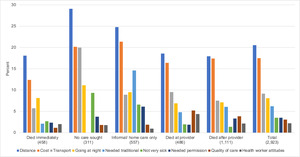
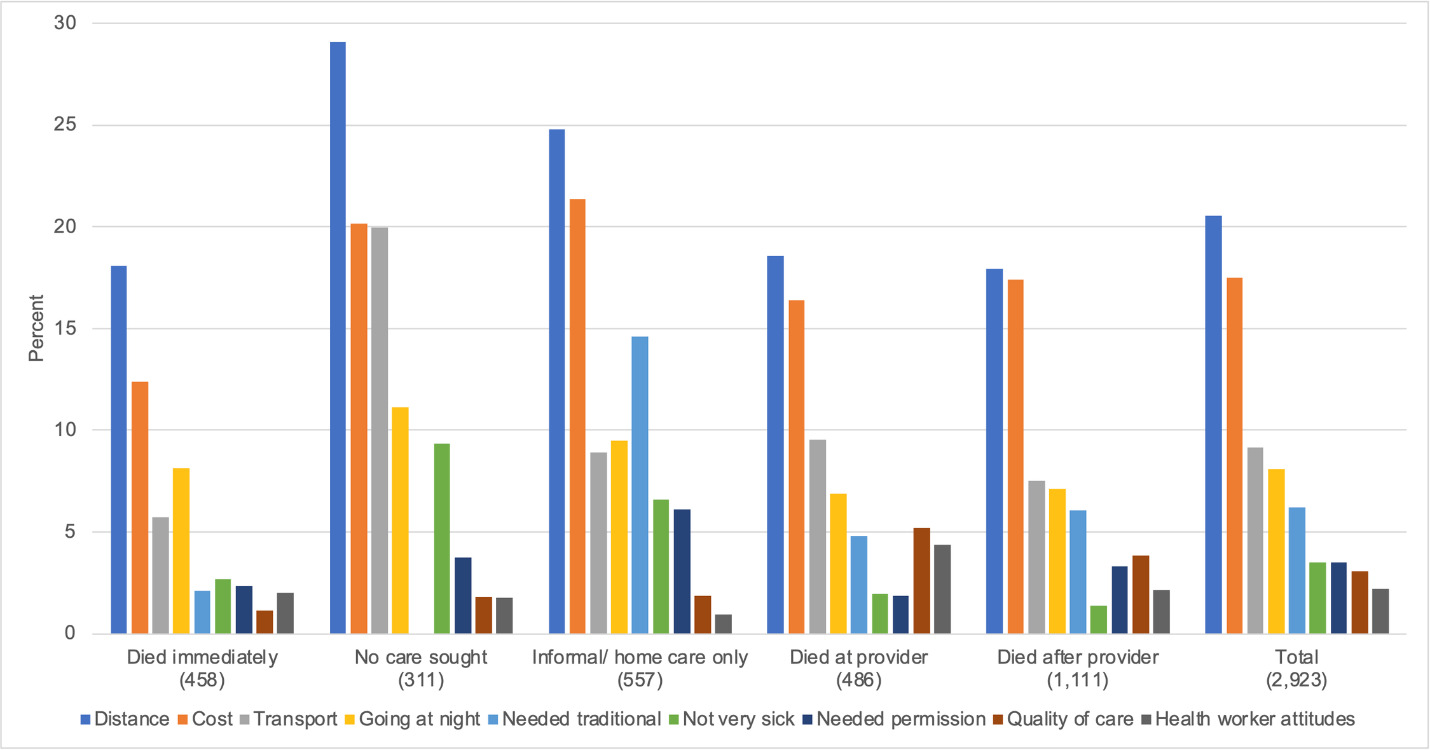
The illnesses were of short duration for children in the “no care sought or received” category. Among neonates in this category, most were home births, and 58% died within one day of becoming ill (mean time to death was 1.7 days), leaving little time to seek or access care in most cases. For children 1-59 months, the median time from illness to death was much shorter in those for whom no care was sought (three days) than in children for whom care was sought (seven days). Looking at barriers to care, the problems of distance, transport, and cost were the highest in this group, as was the belief in some cases that the illness was not severe (Figure 7). The text comments also identified some families who thought of taking the child for care but did not.
Informal care: Home, drug shops, and traditional/spiritual care
Of the remaining 218 neonatal and 1,886 child deaths, 1093 (52%) sought some form of home or informal care either before or instead of formal care. This comprised 598 (28%) home care, 396 (19%) care from a drug shop, and 304 (14%) care from a traditional or spiritual provider (some reported multiple sources of informal care).
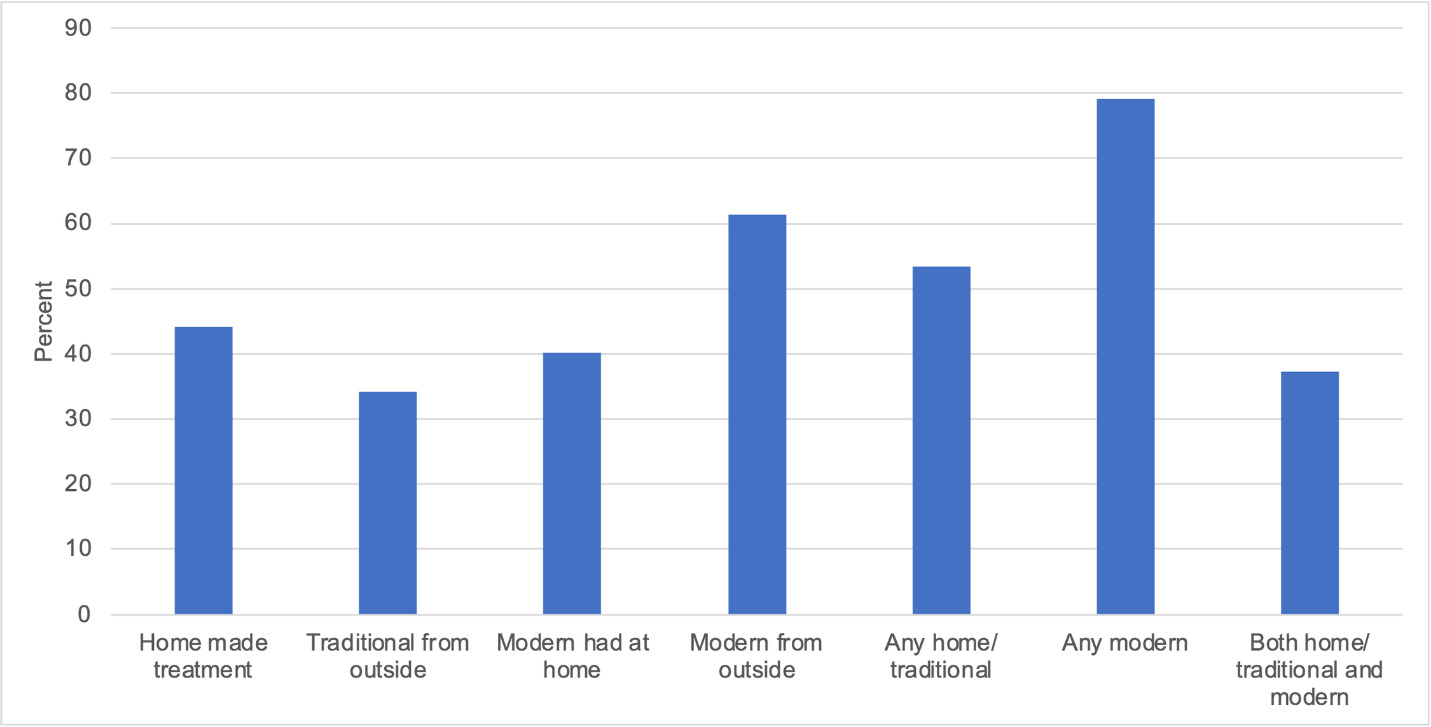
Among home care episodes occurring before any formal care (Figure 8), 79% involved treatment with modern medicines, either available at home or purchased from outside, and/or treatment with traditional medicines (53%), again either prepared at home or purchased from outside, and 37% of the children received both some form of traditional/home remedy and modern medicine as part of home care. Care at traditional providers was sometimes combined with modern approaches, with 16% of such visits reporting receipt of modern medicine (in addition to the traditional or spiritual intervention). Furthermore, 62/218 (28%) and 380/1886 (20%) of remaining neonates and children died after only receiving informal care at home, from drug shops or a traditional/spiritual provider. These comprised 8% of all neonatal deaths and 18% of all child deaths in the study.
The severity of illness and first care
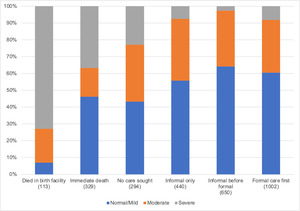
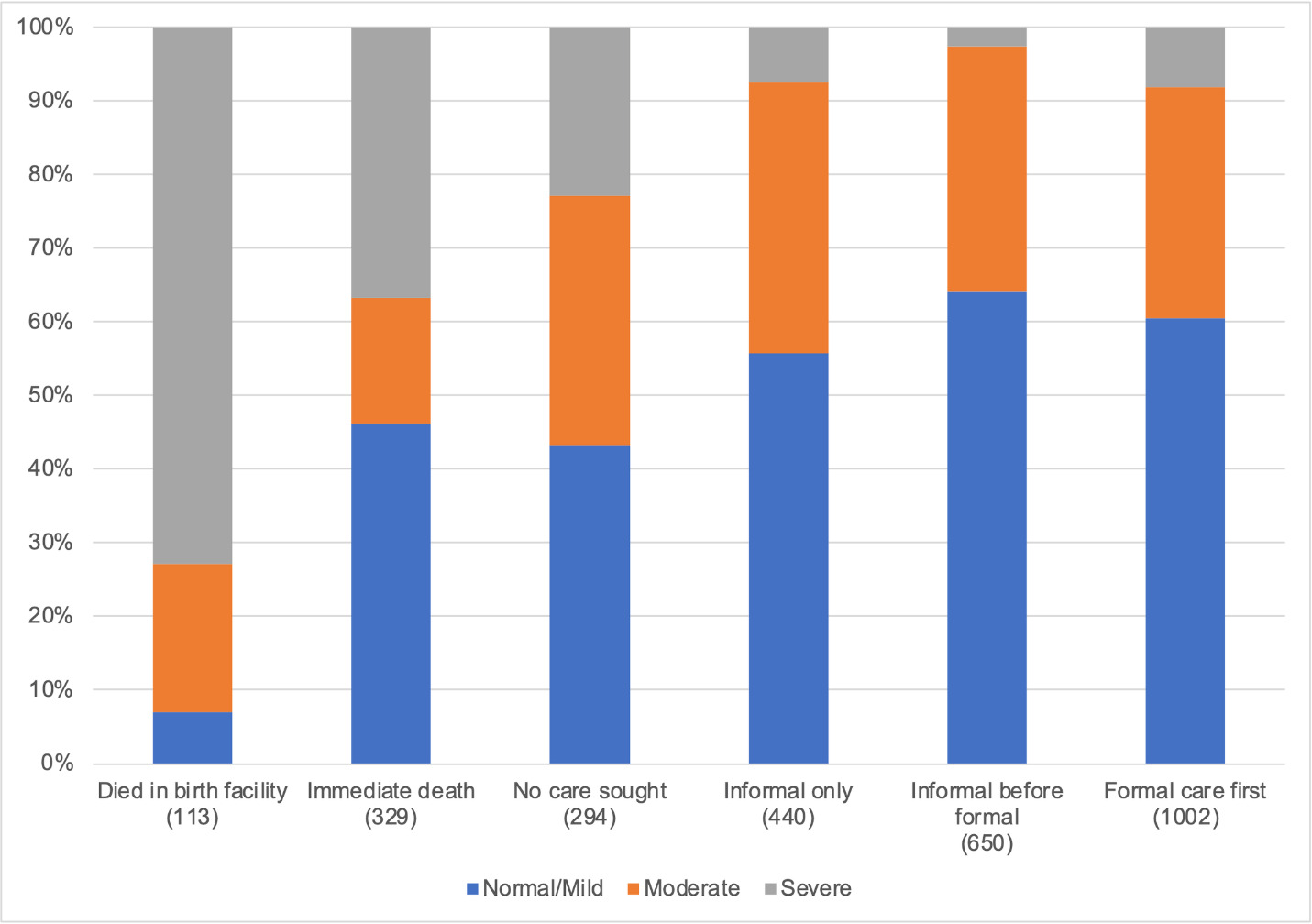
Questions on the child’s feeding, activity, and alertness levels at the time when the illness was first noticed were combined into a three-level scale (scored as 1 = normal-mild, 2 = moderate or 3 = severe) by a method previously described.16 Initial illness severity distribution by the first type of care sought (weighted) is presented in Figure 9.
Newborns who died in their facility of birth before discharge were, for the most part, reported being severely ill. Those at home who died “immediately” consisted of many who were reported to be severely ill (37%), with many others who were said to be healthy or only mildly ill (46%) before dying. Those for whom the caregivers did not seek care included 23% whose caregivers agreed the illness was severe from the start. Both “immediate” and “no care sought” categories were primarily neonates who were mainly born at home and included many newborns with illnesses. About 90% of the informal and formal care cases were child deaths in the 1-59 months age group. All of them were reported to have had mild or moderate symptoms at the time the illness was noticed, although the large group who went straight for formal care as the first action had somewhat more severe illness than those for whom informal care was sought before formal care (8% versus 3% P<0.0001).
Formal care
Formal care was sought for the remaining 155 neonatal and 1,506 child deaths. This is only 25% of the neonates (excluding those who died in a facility before going home), but is 70% of the 1-59 months of age deaths. Of these, 15 (10%) neonates and 101 (7%) children died before setting out or en route to care, leaving 140 neonates and 1,405 children who reached the first provider alive. The most popular type of care providers reached were government hospitals (36%), other government facilities (34%), private hospitals and clinics (16%), health workers in the community (3%), or patent medicine vendors or pharmacy acting as a private clinic (i.e., reported to have examined the child) (10%). Combining public and private hospitals, hospital care was the first formal care received by 43% of families. Average severity was highest for private sector providers (1.73), less for government facilities (1.65) or health workers in the community (1.63), and lowest for drug shops acting as a clinic (1.52). While these show a trend, the difference between individual provider types was insignificant (P=0.195).
Using informal care first may result in delays in seeking formal care. For neonates and children for whom formal care was sought first, the time between first symptoms and the decision to seek formal care was a median of one day and a mean of 1.6 days. For those who used informal care first the median was 2 days and the mean increased to 4.9 days (P<0.0001). Additionally, 32/140 (23%) neonates and 402/1405 (29%) 1-59 months children who reached formal care died at that provider. Those who went to a hospital were more likely to die there (40%) than those who went to another health facility (24%) or to a community level provider (health worker or drug shop acting as a clinic) (2%).
Referral and home instructions
All VASA survey children who left a first formal health provider were still in their final illness. Respondents were asked if the formal provider had referred, or even suggested referral to another provider and whether they provided instructions for home care of the child. Only 13% gave any referral and an additional 18% provided home care instructions, leaving 69% of children with neither. Average severity scores on leaving the facility (1.64) were not improved over the scores when the decision to seek formal care was reached (1.60) (P=0.188). The average for those referred (1.68) was not much higher than those not referred but given instructions (1.62) and those who received neither (1.63) (P=0.570).
Within the text responses there were cases in which the family decided to remove a child from care because the child was not improving and/or they wanted to try traditional treatment. There were even cases in which the provider was reported to have discharged the sick child to go home after no improvement (in one case suggesting traditional medicine for follow up). While these cases are anecdotal, they do suggest some of the complexity of decision making in the sequence of care of children in their final illness.
Additional formal provider visit(s)
Among neonates and children who went home from a first provider in the study, most died at home with no other formal care. This comprised 66/109 (61%) neonates and 575/1002 (57%) children aged 1-59 months. The remaining children made one or more additional visits to a formal provider with 68% of those who had been referred on leaving the first provider reporting an additional visit versus 39% for those not referred (P<0.001). Those not referred but received home care instructions were not more likely to go for another formal provider visit than those that did not. Of the 471 remaining neonates and children for whom additional care was sought, 21 (4%) died before setting out or enroute to the last (usually second) formal provider.
As with the first formal provider, only a minority of deaths occurred at the last provider 69/450 (15%) while the remaining 380 (84%) returned home and died there. Additionally, as with the first provider, the average severity on leaving the second provider was nearly the same as when deciding to go (1.70 compared with 1.72) (P=0.224).
Barriers to care
Caretakers were asked about a list of 12 possible barriers to care, of which the nine most common are presented in Figure 7. The first four barriers (distance, cost, transport, and going at night) were the most frequently reported and relate to access to health services. While these four constraints were mentioned more than others everywhere on the Pathway, they were significantly higher for distance (P=0.002), cost (P=0.032) and transport (P<0.001) among those who did not seek care or used informal care compared to those who used formal care. Though going at night was the fourth most common barrier reported, it was not significantly different between those who sought care and those who didn’t (P=0.148). The four main barriers are particularly prominent among those who did not seek care, or who only used informal care. The next three barriers were factors in the household or community (believing the child needed traditional care, believing the child was not severely ill, and needing permission to go for care). The need to include traditional care was most common among those who sought informal care first (P<0.0001) and second among those who did not seek care at all (P<0.001). Needing permission to go was only reported in 3%, but again was more common in those who only went for informal care (6% P=0.001).
The final two barriers related to the health services themselves, and included the quality of health services and attitudes of health care staff. Although these complaints were not common (3% P=0.002 and 2% P=0.001 overall, respectively) they were more common among those who received provider services.
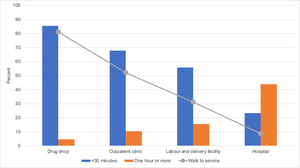
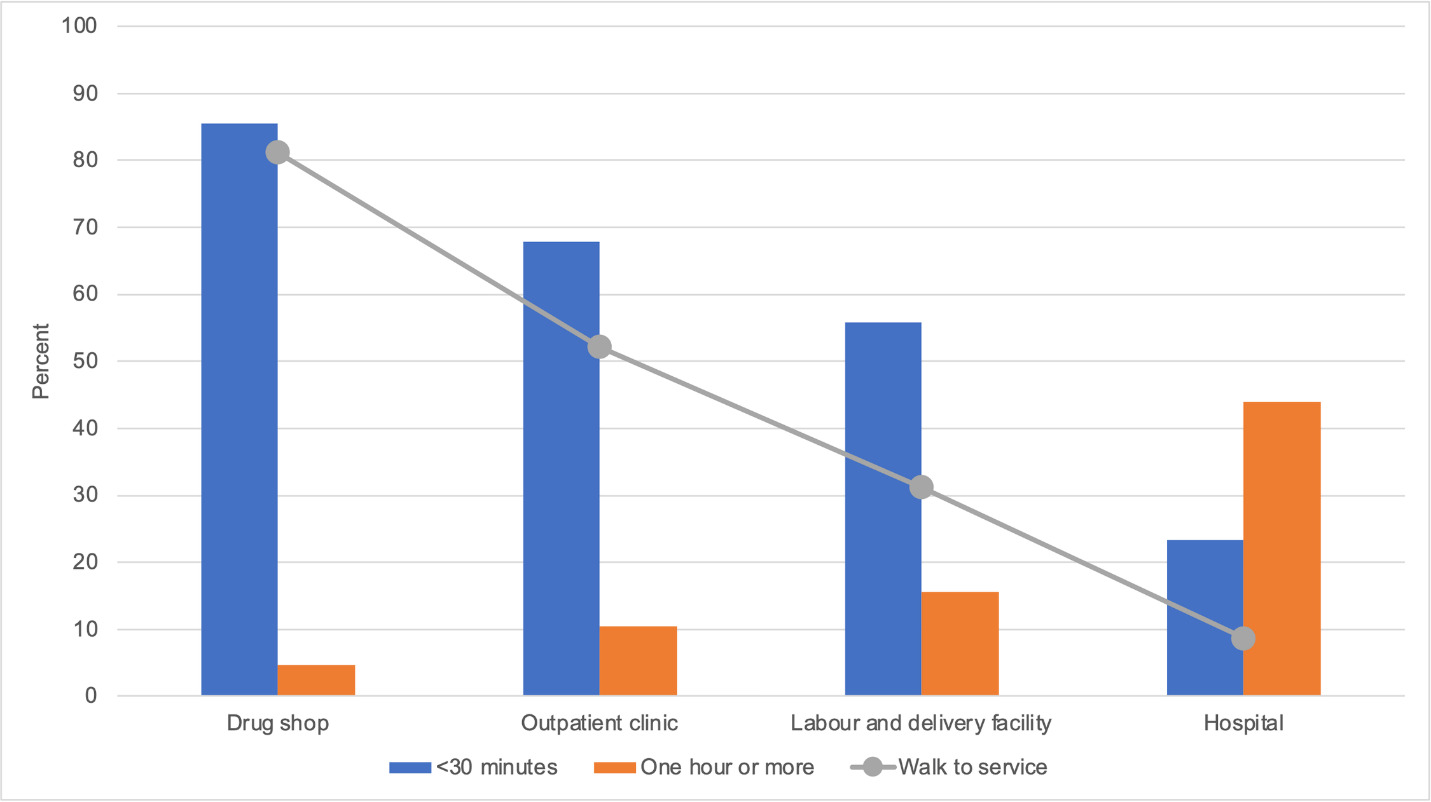
Distance as a barrier to care
In response to the question about travel time and mode of transport to the nearest drug shop (representing informal care) compared to various types of formal cares as shown in Figure 10, most families (85%) with a neonatal or child death noted the distance was within 30 minutes of a drug shop, which would usually be reached on foot (81%). Formal sources of care were increasingly less accessible, with hospital care only being less than 30 minutes away for 23% of families and by walking for only 9%.
Costs as a barrier to care
Cost was the second most common barrier to care mentioned in the VASA survey. Table 4 summarises the percentage of families reporting costs and median costs among those with any cost by type of service. The cost was for both transport and services and included both the cost of a skilled provider at delivery for women with a stillbirth/neonatal death and the cost of care for neonates or children during the final illness. Although the amount families reported spending is small in USA dollar terms, these were significant barriers for poor Nigerian families.
DISCUSSION
Demographics
Child mortality in Nigeria in the 1-59 months age range was strongly associated with levels of wealth and education, both of which were much higher in southern zones than northern zones of the country, and in urban areas than rural areas. The pattern of high mortality for both the youngest and oldest mothers also corresponded with higher rates of early marriage and high fertility in northern zones. The level of maternal education is generally low in Nigeria with about 45% of children under-five having a mother who had never been to school.18 Studies have shown that between 54-66% of mothers of under-five and post neonatal deaths, had never been to school.19 However, the association of these same socio-economic factors with neonatal mortality was much weaker. While there was a significant association with wealth quintiles and geopolitical zones, higher maternal education was not found to be significantly associated with lower neonatal deaths. The socio-demographic characteristics of the children who died in this study are similar to findings from two large population-based cluster-randomised controlled trials in Brong Ahafo, Ghana, which showed that higher maternal education was not significantly associated with lower neonatal deaths.20
Maternal complications, care seeking, and mortality by age group
The maternal care analysis showed that complications in pregnancy and/or labour and delivery were both common and strongly associated with VASA stillbirths and deaths in the first two days. Reducing these deaths requires not only improved quality of care for newborns, but also interventions to prevent or manage these maternal complications. Women with complications, who would otherwise deliver at home, tend to go for facility deliveries, but most facilities in Nigeria are not able to respond to these higher risk cases well enough to bring down neonatal mortality to match levels in the communities. This produces the counterintuitive finding of higher neonatal mortality in facility births compared with home births, which has been observed in other countries and has been attributed to the high facility risk profile.20–22 Studies also suggest that birth facilities that are not able to offer services of sufficient level and quality may have a limited ability to reduce mortality.20 Unfortunately, many women with complications were not able to shift to facility care and so still delivered at home. In Nigeria, there is a need to both increase the accessibility and coverage of obstetric and newborn care and to increase the level and quality of care in facilities to reduce preventable stillbirths and neonatal deaths.
Preventive and newborn routine services
Essential newborn care and preventive services (e.g., immunisation, vitamin A supplementation, and use of insecticide treated nets to prevent malaria) are important ways to reduce newborn and child mortalities. In Nigeria, there are clear gaps in newborn care, including lack of skin-to-skin contact, frequent early bathing, and delayed breastfeeding. These patterns were also reported in the NDHS, which also showed that although care was somewhat better in facility compared with home births, poor newborn care was still common in both locations.3 Immunisation coverage was not reported in the VASA study because the WHO standard verbal autopsy instrument excludes caretaker recall of immunisation and few families had written records. However, the Nigerian DHS shows that coverage of key vaccines was only 27-43% in the high child mortality North West and North East zones, while reaching 71-83% in the lower mortality South East and South West zones. Vitamin A coverage was only 30-31% versus 62-76% respectively in these zones. For these services, the large absolute and within Nigeria gaps correspond to the high mortality rates found. The only exception is in the use of treated bednets which, according to the 2018 DHS, were used much more in the high mortality North West zone (73%) than in other zones (34-47%). Except for bednet use, these gaps in preventive services appear to contribute to the high child mortality rates found in northern Nigeria.3
Nutrition
Malnutrition was not a common primary cause of death in children 1-59 months, but symptoms of malnutrition were commonly reported in the VASA study making malnutrition an important likely underlying factor in the deaths. As with preventive services, Nigeria DHS 2018 rates of moderate and severe malnutrition were much higher in the high mortality zones of the North West and North East.3
Pathway of care
The findings that a substantial proportion (19%) of all neonatal deaths in Nigeria took place in facilities where the child was born and before discharge suggest that improvements in the ability to manage maternal complications and immediate care for sick newborns—that is, the capacity and quality of facility-based care—could reduce this number. Surveys of Nigerian health facilities have found large gaps in both capacity and provider quality.23 The finding that most deaths in newborns and under-fives followed a rapid progression of their illness and were associated with well-known causes suggest that for neonatal cases, the best approach may be the further expansion of access to well-functioning birth facilities and skilled birth attendants, although improved essential newborn care practices in the community may also help. The survey showed that those who faced barriers to early newborn care also faced similar barriers to facility delivery, implying that removing these barriers can be expected to help increase facility births as well as the number of families bringing newborns for care. While informal care in the community was less expensive than formal care, most families spent enough to treat the most common illnesses as has been previously documented.24 The preference for informal care documented in this study was also seen in the NDHS 2018, where treatments for childhood fevers and diarrhoea by patent medicine vendors (PMV) or pharmacies (i.e., drug shops) were more common than in all types of formal health providers combined.3
The most common causes of death for children were malaria, diarrhoea, and pneumonia, all of which can be initially diagnosed and managed at the community level through integrated Community Case Management (iCCM). Nigeria has adopted iCCM as a national policy.25 but it has not been widely implemented. Given the importance of making treatments more accessible and their existing popularity, PMVs and pharmacies need to be considered as possible targets for iCCM training and implementation. Additional analysis of the NDHS 2013 showed that these informal providers frequently acted as more than just drug sellers, with the child being examined in one third of cases and advice on what drug to buy given in another third.26 Whether they can be persuaded to offer appropriate examinations, diagnosis, and treatment advice as iCCM agents is less clear but should be explored and promoted. For newborns the most common causes of death (particularly after the first day or two of life) were severe infectious diseases, and most did not go for formal care. Provision of appropriate care for newborns in the community setting will help to address this challenge of families not wanting to go outside their communities for formal care. As part of effort to address this challenge, Nigeria took part in a study to demonstrate the feasibility of implementing the findings from the AFRINEST study27 within the programmatic setting during which two field sites were established working with the existing health system to provide community-level identification of sick newborns and rapid treatment with simplified regimens from staff at health facilities, either in facility or by outreach to the community.28,29 The implementation research provided Nigeria with a successful tested model for addressing serious infections in newborns in the community that has also been endorsed by WHO.30
Strong components of the preference for informal care were widespread belief in the need for traditional approaches, fatalism, and beliefs regarding spiritual causes of disease. These were explored in depth in the VASA 2019 qualitative study, which has been published elsewhere.31 To a substantial extent, however, families were flexible and improvements in quality and access for modern medical services can be expected to lead to at least a partial shift away from traditional approaches. However, it also makes sense to engage directly with belief systems to encourage good practices respectfully. The lack of significant difference between those who received formal versus informal care based on the scores at the start of illness may be attributed to the failure of families to recognise severe illness in newborns, perceived barriers to care, and the fact that health beliefs may play a stronger role than illness severity in determining actions taken. In many cases, the rapid progression to death also limited the time that families had to decide, prepare for expenses and transport, and go for care.
The substantial number of deaths occurring while preparing for or en route to formal service providers suggests that some families delayed seeking formal care until the child’s symptoms became so severe that they were near death. Earlier effective treatment, whether in the community or easier access and earlier decisions to go to formal health facilities could improve outcomes. Although hospital care was more expensive and more difficult to access, 43% of children who received formal care went first to a hospital. The seriousness of the child’s illness and problems with availability and quality of care in lower-level facilities may have combined with increasing initial use of hospitals when formal care was chosen.
The VASA survey and qualitative study gathered many individual reports of poor-quality care at health facilities, but it was impossible to say how widespread they were from these sources. There are studies focused directly on health facilities in Nigeria that demonstrated widespread gaps in facilities, supplies and provider numbers, types, and capacity.32 These point to the need to greatly improve the quality of care available in many facilities. The low rate of referrals or home instructions for families leaving a formal provider with a child in the final illness was striking, but other VASA surveys in Africa have also noted this problem. However, Nigeria’s referral rate of 13% (and 12% in the Nigeria VASA 2014 for 1-59 months children)13 was even lower than the rates of 18-31% found in VASA studies from Niger, Cameroon, and Tanzania.33–36 Text responses and the qualitative study suggested that families often made decisions about which provider they went to and how long to continue treatment. They took their child home if they thought the child was not improving or was certain to die anyway or if they wanted to try another approach. Furthermore, providers were reported to discharge children who were not improving. The low referral rate of cases documented in this report may be because providers did not think in terms of referral, or that they did not refer if the family was unlikely to go. These same factors may help account for the observation that most children with fatal illnesses who visited a formal provider, including hospitals, did not die there, but returned home to die.
Barriers to care
The main barriers to care found in the study (i.e., distance, cost, transport, and travel at night) also relate to each other, with more distant facilities usually requiring vehicle transport, which is itself expensive for poor families. Travelling for an emergency at night was even more demanding in terms of finding and paying for transport as well as problems with insecurity. As was found in the section on travel to care, only drug shops were readily available to most families on foot, so it was not surprising that they were often favoured as a source of care.
Table 4 (cost as a barrier) showed that despite some states in Nigeria declaring a policy of free care for maternal and child health, it was uncommon for care at a formal provider to be free (7-8%). In qualitative comments, additional cost barriers for going to formal providers are that families need to bring substantial funds when they set out since they might have to pay a deposit before care is given and that the total cost was not only high but also unpredictable (as evidenced by the wide inter-quartile range) making it difficult for some families to commit to this level of care. On the other hand, while informal community services were usually not free, they were less expensive, and some community providers were reported to be willing to provide services on credit, making them financially much more accessible.
Other barriers were not commonly reported but contributed to caretakers’ problems accessing quality care for sick children. Individual text responses and the qualitative study included reports of facilities being closed due to staff absenteeism, strikes or insecurity, poor attitudes of staff towards patients, and facilities not being able to provide care due to lack of medicines or other supplies.
CONCLUSIONS
The 2019 VASA study identified family, community, and health system factors related to neonatal and child mortalities in Nigeria. It was common for several factors to be present at once for the deaths and can each contribute to the sequence of events resulting in a preventable death. These common factors could interact and reinforce each other. If a family did not receive preventive services and did not have affordable access to good quality curative care, their child may have been more likely be malnourished and fall ill more often, and the family may have turned more to traditional and home care, risking delayed and ineffective treatments. On the side of the healthcare system, community-level care can be improved by increasing outreach and coverage of preventive services and by bringing quality curative care to the community (through Integrated Management of Childhood Illness, Integrated Community Case Management of Childhood Illness and Community Management of Possible Severe Bacterial Infections in Newborns). Community care needs to be complemented with good quality primary health care and some secondary facilities able to handle more severe cases and offer maternal care at a level high enough to substantially impact newborn deaths (e.g., basic or comprehensive emergency obstetric care). Improved health services would improve trust and utilisation, but there may also need to be direct engagement with family beliefs to encourage better care for mothers and childhood illnesses.
Acknowledgements
The authors wish to express their profound gratitude to USAID-CIRCLE Solution for their financial and technical support throughout the entire process of the study. Our gratitude also goes to the NPC, FMOH, NPHCDA, NBS, and Ministry of women affairs as well as the field team and other relevant stakeholders who contributed towards the successful completion of the study. The valuable contribution of the mothers/caregivers of the deceased children, are hereby deeply appreciated. Their cooperation during the field work/data collection were the key to the successful generation of the data for this study.
Disclaimer
The views are those of the authors and not necessarily those of USAID.
Funding
The 2019 Nigerian VASA study was supported financially by the United States Agency for International Development (USAID) through the CIRCLE project.
Authors contributions
Data curation and analysis: George Ikechi Eluwa, John Quinley
Field investigation: Robinson Daniel Wammanda, John Quinley, George Ikechi Eluwa, Michael Kunnuji, Inuwa Bakari Jalingo, Olorunimbe T Ayokunle, Alice Romokek Nte, Rebekah King, Ana Claudia Franca-Koh
Writing (original draft): Robinson Daniel Wammanda, John Quinley
Writing (review and editing): Robinson Daniel Wammanda, John Quinley, George Ikechi Eluwa, Michael Kunnuji, William Weiss, Inuwa Bakari Jalingo, Olorunimbe T Ayokunle, Alice Romokek Nte, Rebekah King, Ana Claudia Franca-Koh.
Competing interests
The authors completed the Unified Competing Interest form at http://www.icmje.org/disclosure-of-interest/ (available upon request from the corresponding author), and declare no conflicts of interest.
Correspondence to:
Wammanda Daniel Robinson. MB, BS. FWACP(Paed)
Department of Paediatrics, Ahmadu Bello University Teaching Hospital, Zaria Kaduna state, Nigeria.
Email: [email protected]