Shoulder to Shoulder Global (STSG) is a global health initiative seeking to improve the health and well-being of impoverished and underserved communities worldwide. In Santo Domingo, urban crowding has resulted in the formation of cooperativas or barrios generally located on the outskirts of the city.1 Many of these communities lack electricity, developed water sources, sanitation, and access to healthcare.2 In 2002, STSG established partnerships with community health organizations in the area to work toward a sustainable impact on healthcare. Nearly two decades have passed and STSG has grown exponentially. In 2007, a clinic, Centro de Salud Hombro a Hombro (CSHH), was opened in the cooperativa of Carlos Ruiz Burneo to provide primary care, pharmacy services, oral health services, and preventative health workshops to the surrounding area.1 The Fundación Hombro a Hombro was established with US and Ecuadorian board members to enact financial operations on behalf of CSHH. In line with its vision to support the local community, the foundation employs local staff at the CSHH with the support of STSG to provide healthcare to nearly 50 patients per day. The clinic serves about 20,000 people from the barrios of Carlos Ruiz Burneo, Plan de Vivienda, and Luz del Dia.
While the CSHH has served the community for over a decade, STSG continues to provide support to the clinic in the form of interprofessional short-term experiences in global health (STEGHs). Interprofessional STEGHs began in 2008 with the aim to provide acute care to patients and refer more extensive or chronic health problems back to CSHH.1 Additionally, STSG partnered with Timmy Global Health (TGH) which provided monetary, technologic, and human capital support to the STEGHs. Throughout each academic year, health professionals and students from communication sciences and disorders, dentistry, education, Hispanic studies, medicine, nursing, pharmacy, physical therapy, physician assistant studies, psychology, and public health travel to Santo Domingo, Ecuador for STEGHs in March, May, June, and August.1 The STEGH teams work together to supplement existing healthcare efforts to patients across various sites in Santo Domingo and the surrounding area. In 2010, TGH implemented an electronic medical record (EMR), TimmyCare (Timmy Global Health, Indianapolis), in the CSHH clinic, which is also used by the STEGHs. Through the use of a local intranet, TimmyCare allows clinic staff and STEGH volunteers to follow a patient from registration at reception to discharge at the pharmacy. The implementation of an EMR has allowed for improved efficiency, accuracy of patient care, and systematic data inquiry for research purposes.
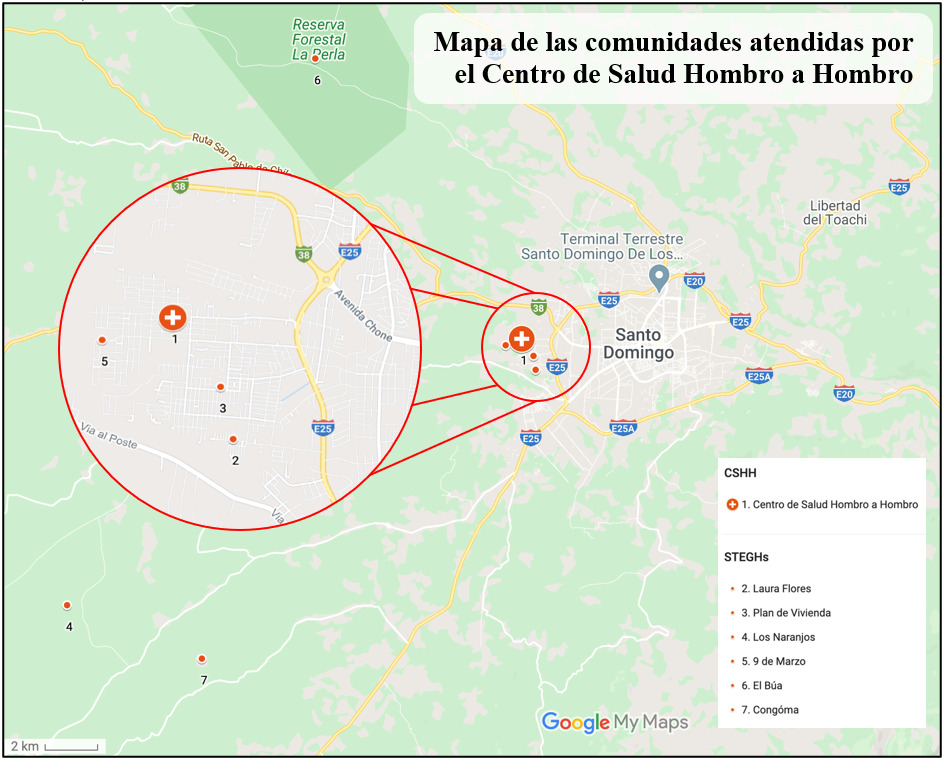
A large majority of patients served by CSHH present from peri-urban communities. As STSG has continued to develop, CSHH has formed partnerships with the indigenous Tsáchila people who live in small, isolated rural communities outside city limits with little access to healthcare (Figure 1).1 However, through partnerships with Tsáchila community leaders, STSG and TGH are able to reach these communities at least three times per year to provide health services. While the STEGHs provide health screenings and healthcare to patients in the community away from the clinic, the goal is to establish relationships with these patients and refer them to CSHH in order to provide care for chronic conditions and improve continuity of care. Despite these efforts, many patients presenting to the STEGHs from the Tsáchila communities continue to report that their only access to healthcare is via STEGH.1,3 With the assistance of STEGHs, the CSHH has realized one of the most common chronic diseases for the people of Santo Domingo and the Tsáchila community is anemia.
Globally, anemia is considered the most common nutritional deficiency affecting approximately a quarter of the world population, especially children and women of reproductive age.4 Iron deficiency is one of the most common causes of anemia.4 Severe anemia is associated with fatigue, weakness, dizziness, and drowsiness.5 Pregnant women and children are most vulnerable to the deleterious effects of anemia. For the developing fetus, major risks of anemia include preterm birth and low birth weight.4,6 In children, anemia can negatively affect cognitive development, school performance, growth, and immunity.7 According to the World Health Organization (WHO), Ecuador is classified as moderate to severe with regard to level of public health significance for anemia.5 Per the WHO, the estimated percentage of Ecuadorian children, non-pregnant women, pregnant women, and all women of reproductive age with anemia are 40%, 24%, 29%, and 24%, respectively.5 The Ecuadorian Ministry of Health provides classifications for anemia.8 However, this guide only includes anemia ranges for pregnant women that coincides with the guidance from the WHO.8,9 However, these country-level data are insufficient to develop a targeted anemia intervention strategy in the communities served by STSG and CSHH.
While STSG continues to aid the CSHH by allocating funds and other resources for nutritional supplements, little has been done to characterize specific risk factors for anemia in this population. Previous efforts to improve anemia via iron supplementation have been unfocused with questionable evidence of benefit. The objective of this study is to provide demographic information for the anemic population and determine specific risk factors for anemia at STSG STEGHs and the CSHH clinic in order to take actionable steps for iron supplementation or other interventions in the future. It is hypothesized that higher incidence rates for anemia will be seen among women and subjects from indigenous communities.
METHODS
Population
This retrospective, cross-sectional study was declared exempt by the University of Kentucky Institutional Review Board. Due to limited resources and cost considerations for the CSHH, only subjects from 1 to 6 years of age, female subjects greater than 12 years of age, or any subject with clinical signs of anemia were routinely screened in accordance with standard clinic protocol. In order to determine anemia status, hemoglobin (Hgb) levels were measured via capillary blood obtained with one-way lancets fitted to an ACCU-CHEK® lancing device (Roche; Mannheim, Germany) and analyzed using portable HemoCue Hb 201+ hemoglobinometers (HemoCue America; Ängelholm, Sweden). If Hgb levels were unattainable due to instrument malfunction or maintenance, hematocrit (HCT) concentrations were obtained. All HCT concentrations were converted to Hgb equivalents for data analysis by dividing the HCT concentration by three.9 Subjects were considered anemic if they met mild anemic status with hemoglobin levels consistent with the WHO Anemia Definitions for their age group and, if adult, sex.8,9 Subjects were grouped into their respective communities from which they presented to the STEGH or the CSHH. Duplicate patient information after the first encounter was removed by excluding duplicate subject encounters.
Measures
To extract the data, TimmyCare was queried for patient demographics, including patient and visit identification number, age, sex, pregnancy status, and community location. The seven community locations included Laura Flores, Plan de Vivienda, CSHH, Los Naranjos, 9 de Marzo, El Búa, and Congóma. The communities of Los Naranjos, El Búa, and Congóma are predominantly comprised of indigenous Tsáchila people and located furthest from the CSHH (Figure 1). TimmyCare assisted in harvesting further information pertinent to anemia diagnoses, including Hgb level or HCT concentrations. Data from all subjects who received Hgb or HCT testing from January 1, 2010 to August 31, 2016 were compiled. No subjects were excluded based on age, sex, or race.
Statistical analyses
Univariable and bivariable analyses were conducted using Chi-squared tests or Fisher’s exact tests, when appropriate, to describe the distribution of subject characteristics. Demographic characteristics, location, and year at data collection were considered in the analysis. Odds ratios (OR) and 95% confidence intervals (CI) were calculated via logistic regression. Logistic regression analysis to identify factors associated with anemia was conducted with SAS software version 9.4. Backward elimination was used to generate the final predictive model. In addition, a stratified analysis was conducted to evaluate whether factors associated with anemia differed by sex.
RESULTS
Data from a total of 1328 subjects were collected, which reflects all subjects with hemoglobin levels recording during the study period. Of the 1328 subjects initially screened, 1145 (86.2%) were unique subject encounters. Within the unique subject population, 67.2% were female, 33% were children under five, 1.6% were pregnant, and 42.8% were anemic. Over 42% of anemic subjects were younger than the age of five compared with only 26% of non-anemic subjects. Subjects were distributed throughout the seven communities with 11.2% presenting from an indigenous community. Demographic characteristics of the study population are further summarized in Table 1. Figure 2 depicts row percentages for each of the variables tested in this study for anemia in order to demonstrate the effect of anemia within each group. When subjects with anemia were compared to subjects without anemia via Chi-square analysis, a statistically significant result was seen for age group (p<0.001) and location (p<0.005).
The final logistic regression model generating the odds ratios of anemia with a number of covariates including age, sex, pregnancy status, and community location is included in Table 2. The subjects from Congóma were excluded from the logistic regression due to the low sample size for this location (n=5). The youngest subjects (<5 years of age) had 1.46 times the odds of anemia compared to the oldest age group (>15 years of age) (95% CI [1.17, 1.82]). Additional groups with greater odds for anemia presented from the communities of Plan de Vivienda (OR = 1.36; 95% CI [1.09, 1.69]), Los Naranjos (OR = 1.5; 95% CI [1.04, 2.17]), or El Búa (OR = 1.61; 95% CI [1.12, 2.32]). Neither female sex (OR = 1.02; 95% CI [0.83, 1.25]) nor pregnancy status (OR = 1.25; 95% CI [0.61, 2.54]) were statistically significant for anemia per the model (Table 2). Additionally, age groups 2 and 3 had lower odds of anemia. However, neither age group 2 (OR = 0.94; 95% CI [0.72, 1.23]) nor age group 3 (OR = 0.84; 95% CI [0.53, 1.32]) were statistically significant the per the logistic regression model.
When controlling for male sex, the first age group (<5 years of age) had 5.61 times the odds of anemia compared to the oldest age group (>15 years of age) (95% CI [2.62, 12]). Only one location yielded statistically significant odds of anemia within the male population, Plan de Vivienda (OR = 1.77, 95% CI [1.03, 3.04]). Similar results were reflected in the female population as well resulting in 1.48 times the odds of anemia in the first age group compared to the oldest age group (95% CI [1.03, 2.13]). Females presenting from Los Naranjos and El Búa had statistically higher odds of anemia when compared to CSHH (OR = 2.27, 95% CI [1.2, 4.31] and OR = 2.5, 95% CI [1.36, 4.63], respectively). Among the female subgroup analysis, pregnancy status was not a statistically significant predictor of anemia (OR = 0.72, 95% CI [0.27, 1.93]. Given a lack of statistically significant prediction for anemia in the pregnant female population, additional analyses were performed. After reconfiguring the model to exclude male subjects, pregnancy was again not a statistically significant predictor of anemia (OR = 1.39, 95% CI [0.52, 3.71]).
DISCUSSION
To the knowledge of the authors, this is the first study to investigate risk factors for anemia among subjects living in Santo Domingo, Ecuador, and the public health implications for risk-related factors. Several risk factors were found to be associated with anemia in this population. Subjects greater than five years of age were less likely to be anemic than subjects less than five years of age. This finding is consistent with WHO anemia estimates for Ecuador in 2011.5 Although a large proportion of the study population was children, the adult male group likely reflects an element of selection bias within this study.
This study demonstrated that males were more likely to be anemic than females. However, sex was not a statistically significant predictor of anemia in the logistic regression model when adjusting for additional factors. According to the WHO, all Ecuadorian women of reproductive age are at moderate risk of anemia.5 Large demographic differences and potential selection bias in this study could account for the apparent reduced risk of anemia for females in this population. Due to standard clinic and STEGH procedures, only subjects from 1-6 years, only female subjects ≥12 years, and any other subject with clinical concerns for anemia are screened for anemia. Given that women of reproductive age are frequently provided nutritional supplementation via prenatal vitamins, females may have an artificially diminished prevalence of anemia. Due to this potential selection bias, male subjects with a higher clinical suspicion for anemia may have been tested with greater frequency resulting in a falsely elevated prevalence of adult male anemic subjects. Despite more females being routinely tested, including a large majority of females who have a high clinical probability of testing positive for anemia, selection bias may account for the inability of the study to demonstrate female sex, a known risk factor for anemia, as having a higher risk of anemia.4
Pregnancy was also not a statistically significant predictor of anemia in this study. A higher incidence of anemia in this population was expected due to gestational iron demands for fetal development.4 However, prenatal supplement use and/or low sample size in this population may have affected the lack of statistical significance in this study. Although STSG provides prenatal vitamin supplementation to patients during clinic visits and STEGH encounters, the extent and impact of these interventions are unknown. Despite this, up to 85% of Ecuadorian women access prenatal healthcare less than once per month throughout pregnancy.10 Given these results and the relatively small number of pregnant subjects in this study, it is difficult to draw conclusions from this population. Additional studies are required in order to determine the relationship between anemia and specific risk factors for this population.
Location was a statistically significant predictor of anemia. Presenting from the communities of Plan de Vivienda, Los Naranjos, or El Búa was associated with higher prevalence of anemia. Although subjects from indigenous Tsáchila communities only comprised a small proportion of the total population (11.2%), Los Naranjos and El Búa accounted for two of the three communities with higher risk of anemia. These communities are more rural, often several miles from community centers, and lack access to proper nutrition and routine healthcare.3 In contrast, Plan de Vivienda is one of the most proximal community locations to CSHH. When selecting a site for the CSHH, communities were anecdotally assessed by STSG founders based on which communities might have the highest level of health disparity. Based on health disparity and many other logistical factors (eg, centrality of the clinic to other locations within the community, ease of access for STEGHs, etc), the CSHH was strategically placed in an area that might benefit most from additional healthcare services. The poverty within this community severely limits access to basic resources, such as nutritious food and clean water. Due to the proximity of this community to CSHH, subjects from Plan de Vivienda may be over-represented in this sample because of the ease of access to the various STSG and TGH STEGHs. Previous work with CSHH shows approximately 33% of children in the first age group had evidence of developmental stunting as evidenced by height-for-age Z-scores of -2.0 or worse (29 of 89 children), around 50% of preschool children had stunting, and 25% had wasting (low weight-for-age).3 While growth stunting can be caused by low birth weight, other factors such as parasitic infection can play a role in development.11 Although additional research is required to clarify the relationship between parasitism and anemia in these communities.
Limitations
This study has several limitations. First, data input into TimmyCare during patient registration could have potential errors because there are many volunteers who assisted with registration of subjects during STEGHs and at CSHH. Additionally, due to the non-profit nature of STSG and TGH, laboratory collection resources are limited and many adult subjects, particularly men, who received blood testing for anemia may have had other symptoms of anemia, such as fatigue, and been referred for testing by a healthcare provider after preliminary examination. This could have introduced a significant degree of selection bias into the study. With regard to laboratory testing, subjects received HCT and Hgb testing due to limitations of available instrumentation. Due to instrument maintenance and potential for laboratory error in the clinic, it is possible that some HCT concentrations or Hgb levels were falsely reported. Additionally, there is data to suggest that it is impossible to accurately convert HCT to Hgb, which may have resulted in false reporting of anemia in subjects with only HCT results.12 However, the conversion method described has been historically accepted and is standard practice within the clinic and on STEGHs. Additionally, only 49 data points (4.1% of the sample) required conversion from HCT to Hgb. This study is based on a convenience sample of subjects within close proximity to the CSHH in Santo Domingo, Ecuador in addition to the more remote Tsáchila communities. Thus, these results are not generalizable to a larger population in Ecuador. Despite these limitations, this study identifies risk factors associated with anemia in this population that may allow STSG and its partners to make more mindful pharmacotherapeutic and/or dietary interventions in the future.
Anemia is an important public health issue due to potential adverse effects on maternal and child health and development.4 There is little published research on geographical implications on anemia in low- and middle-income South American countries, although there are likely to be important public health implications of anemia given the high prevalence and the possible additional effects of poor diet or parasitic infection. Public health recommendations include increasing access to sufficient iron supplementation and providing health education messages that increase awareness of the potentially adverse nutritional consequences of poor diet.13 Public health policies aimed at improving rates of anemia should continue to support programs that provide iron supplementation and/or improve access to iron-rich foods.
CONCLUSIONS
In summary, this study identified two risk factors for anemia in this population. Age less than five years or residing in three of the observed communities were predictive of anemia. These findings are of public health relevance and will be the focus of greater targeted pharmaceutical and educational efforts for STSG in the future. Although there were many limitations to this study, especially potential selection bias, the overall concept will assist in the formation of a uniform strategy to develop education and intervention programs to reduce the prevalence of anemia in these populations in Santo Domingo. Health education programs led by the CSHH and STEGHs should be explored as an entry point to decrease the burden of anemia in peri-urban and rural areas of Santo Domingo.
ACKNOWLEDGEMENTS
The authors would like to thank the CSHH staff for allowing their clinic to serve as a research site. Additionally, the authors extend special thanks to Craig Borie and Pablo Boada for coordinating STEGH operations to allow for this study to be made possible. Thanks to Timmy Global Health for their partnership and support of the various STEGHs and initiatives in Santo Domingo, Ecuador throughout the years. The research presented in this paper is that of the authors and does not reflect the views of the University of Kentucky. Kevin Mercer was responsible for leading study design, data collection, and manuscript production. Daniela Moga, Steven Fleming, Wayne Sanderson, and Melody Ryan assisted with study design, analysis of statistical tests and results, and manuscript revision. No financial disclosures were reported by the authors of this paper. The results of this study were in part presented at the American College of Clinical Pharmacy Global Conference on Clinical Pharmacy Conference in October 2018. Additionally, these findings have been published as part of a Master of Public Health capstone submission for the University of Kentucky College of Public Health.
FUNDING
No funding was provided for this research. No financial disclosures or other conflicts of interests are reported by the authors of this paper.
AUTHORSHIP CONTRIBUTIONS
KJM: Conceptualization, Methodology, Software, Formal Analysis, Investigation, Data Curation, Writing – Original Draft, Writing – Review & Editing, Visualization, Project Administration
DM: Methodology, Software, Formal Analysis, Writing – Review & Editing
SF: Conceptualization, Methodology, Writing – Review & Editing
CC: Resources, Writing – Review & Editing
MHR: Conceptualization, Methodology, Validation, Writing – Review & Editing, Visualization, Supervision
COMPETING INTERESTS
The authors completed the Unified Competing Interest form at http://www.icmje.org/disclosure-of-interest/ (available upon request from the corresponding author), and declare no conflicts of interest.
CORRESPONDENCE TO:
Kevin J Mercer, PharmD, MPH
Department of Pharmacy, Memorial Hermann Memorial City Medical Center, 921 Gessner Dr, Houston, TX 77024
[email protected]