In 2015, the Joint United Nations Programme on HIV and AIDS set the 95-95-95 targets with the goal of having 95% of people living with HIV (PLHIV) tested, 95% of those testing positive initiated into care and treatment, and 95% of those on treatment virally suppressed by the year 2030.1 Viral suppression for PLHIV is essential to maintaining their health and, when the virus is suppressed to undetectable levels, HIV is not transmittable to others.2 Viral suppression is achieved through adherence to effective anti-retroviral drugs (ARVs) and is most effectively monitored through viral load (VL) testing.3,4 Achieving widespread VL testing coverage is critical to reaching the third 95% goal; yet, hurdles in scale-up of VL testing persist in remote regions3–6 where transportation of VL samples is challenging and turnaround time (TAT) for VL test results is high.5 One potential solution to decrease TAT is the use of unmanned aerial vehicles (UAVs), or drones, to transport VL samples and ARVs.7
Interest in UAVs for transport of laboratory specimens and medical commodities has grown in recent years, and UAVs have been used to routinely transport medical supplies in a few countries. 7–11 However, limited evidence exists on the cost of using UAVs for routine transport of laboratory specimens which require landing at remote clinics to pick up samples (termed directional transport). Additional questions remain about the feasibility of UAV services that are purchased through a logistics company, as opposed to a country or program purchasing and operating the units themselves, and when the distances required for transport are farther than 100 kilometers.
Determining the cost to utilize UAVs for routine transport of specimens is difficult considering the multiple assumptions that must be accounted for, including the type of UAV and the associated operational costs. A nationwide study in Liberia12 determined that fully replacing the motorbike transport program with UAVs for lab samples would be more expensive to operate. Phillips et al.13 conducted a costing analysis that compared UAV-based systems to ground-based for the transport of laboratory samples from health facilities to labs in Malawi and found higher costs but lower travel times when using small, battery-powered UAVs for transport. Haidari et al.14 modelled the feasibility and cost of using UAVs to transport vaccines in Mozambique, finding that for distances under 75km, UAVs increased availability of vaccines and decreased logistic costs. Others have studied how small UAVs might improve lab specimen transport over short distances.15–17 While these research activities are informative, their findings are not transferable to settings which require UAVs to fly longer distances with heavier cargo, and when UAV services are purchased from a third-party logistics company. Furthermore, UAV technology is progressing rapidly, and the UAVs that will soon be ready for commercial use can transport larger quantities over greater distances making them potentially more useful for last-mile logistics in remote locations.
Specimen transport in Turkana County, Kenya
Turkana County is a large rural and remote area in northwest Kenya. The Afya Nyota ya Bonde project (Afya), a 5-year USAID-funded project implemented by FHI 360 (2018 – 2022), is improving the capacity of commodity management and strengthening the laboratory network services for VL testing in order to reach the 95-95-95 targets. The Afya project supports 18 health facilities in Turkana County, 15 of which are in rural areas beyond the main town of Lodwar, the largest urban area in the county. Effective service delivery for PLHIV in Turkana County is hindered by several factors affecting transportation: underdeveloped road networks and unpredictable flash floods18; insecurity and violence19; vast distances between health facilities that offer HIV care and treatment services and the central laboratory where samples are tested; and unreliable transportation options.
Currently in Turkana County, health workers are responsible for transporting VL samples from their health facility to Lodwar, where the average one-way trip takes 4.5 hours. A courier service then transports the samples to a national reference laboratory in Eldoret, about an 8-hour drive one-way. All facilities collect VL samples using dried blood spots (DBS), drops of blood dried on filter paper packaged in an envelope for transport. Similarly complex is the distribution of ARVs. The Kenya Medical Supplies Authority (KEMSA) currently transports ARVs from national warehouses to Lodwar; then healthcare workers from around the county must travel to Lodwar to pick them up monthly. The challenges of transportation in this county severely impact service delivery: ARVs are often delayed reaching health facilities, and VL samples are delayed reaching the laboratory; with only 3% of all samples currently meeting the goal of a TAT less than four days. These delays prevent patients from receiving timely, clinically-informed therapies.20 Additionally, when health facility staff are away transporting VL samples and retrieving ARVs, provision of health services can be interrupted as small facilities must close when their one health care worker leaves.
The National AIDS/STD Control Programme (NASCOP), operated by the Kenyan Ministry of Health, records three segments of the total turnaround time for a VL sample: (1) the time between the collection of the sample from the patient to when it is received at the laboratory; (2) the time between the receipt of the sample at the laboratory until it is processed; and (3) the time between processing and dispatching the result. For the Afya Project, the ideal turnaround time for the first segment, referred to as TAT-1 in this text, is under four days. Official NASCOP data was available for 11 of the 15 remote health facilities in Turkana between January and March, 2018, the period immediately prior to the start of Afya project, and shows the TAT-1 for all 270 VL samples taken during this time averaged 13 days (range 1-30), with 97% of VL samples arriving four or more days after the sample was drawn. We used data prior to the start of the project as it was a realistic TAT without project support that was financially and logistically not sustainable by the Ministry of Health.
Study objectives
Given the current transportation challenges faced in Turkana County, we aim to estimate the costs and potential time savings to the health system by replacing or supplementing ground transport of VL samples and medical commodities with transport by UAV. We model several different transportation scenarios at Afya-supported health facilities in Turkana County. For each scenario, we assess the potential costs and reduction in TAT-1 as compared to the current transportation system. Our results are intended to inform government officials and decision-makers considering UAVs for transportation of commodities, as well as UAV manufacturers and logistics companies interested in using UAVs for this sector.
METHODS
This modeling study employed secondary analyses of health facility data, and de-identified data on the turnaround time for VL specimens. The study was reviewed by FHI 360’s Office of International Research Ethics and was deemed to be a non-human subjects research activity. Use of programmatic data was approved by the Afya project as well as the Government of Kenya.
In this section, we discuss the assumptions of current practices, the data inputs we used for modeling the transportation network and informing the assumptions, and the logistical needs for UAV that was used to model transport scenarios. We then describe the modeling process for costing the current transportation system and the UAV transportation scenarios.
Data sources
We combined data from a national health database, health facility logs, and open-source spatial data. De-identified VL laboratory sample data were provided by NASCOP to determine sample origin and TAT for the Afya-supported health facilities. Data on the number of trips taken by health care workers to transport samples for VL testing, early infant diagnosis (EID) of HIV infection, TB, and others to Lodwar were collected by Afya staff from facility transportation logbooks. Facility locations in latitude and longitude were provided by the Afya project and were validated and corrected using satellite imagery from Google maps. The road network was downloaded from OpenStreetMap®.21 A UAV flight path network was created in ArcGIS,22 a geographic information system (GIS), by creating straight-line routes between all facilities. Average costs for ground-based transportation between health facilities and Lodwar town (including the staff per diem and the private transportation fare), and costs for the courier service from Lodwar to the laboratory were provided by the Afya project based on the local transport rates within Turkana. Estimated costs for UAV-based transportation and UAV specifications were provided by a logistics company in Kenya that is planning to add UAVs to its fleet.
Assumptions
Transport scenarios were developed and modeled to compare cost and TAT for different transport method configurations. The scenarios are based on the following assumptions regarding the current methods of transporting VL samples and ARVs, and UAV specifications (Table 1). For this modeling exercise, we used an average setting for the system; the parameters are explained in this section, and the resulting averages for each variable are presented as results in Table 2.
Currently, VL tests are not consolidated into weekly or monthly designated VL testing days. Instead, health workers provide VL testing services to antiretroviral (ART) patients as they are seen at a facility. This requires providers to either hold the VL samples until they accumulate enough to warrant transport to Lodwar, thus delaying TAT-1, or to travel to Lodwar after each day when tests were drawn from the patient, increasing the travel frequency, transportation costs, and provider time away from the facility. For UAV transport to be cost effective, however, we modeled consolidated VL testing days to reduce the number of flights. A UAV would be scheduled to pick up the VL samples the day after the ART patient is seen, which will also help reduce TAT-1. As the algorithm in the national guidelines23 provides the ART client with a 60-day window around the due date for their next test, each facility should offer at least one VL testing day per month. This will ensure each ART patient has at least two opportunities to access VL testing within their window.
In order to extrapolate data from logs and the NASCOP database on VL samples, which were used to model our scenarios, we generated three key variables.
-
Expected number of VL samples per month, by facility: According to Kenya’s national HIV testing algorithm, new clients require one VL test for every six months in their first year. Virally suppressed clients require one VL test per every 12 months; and non-suppressed clients require testing once every three months until they are virally suppressed. We assumed non-suppressed clients require two tests in 12 months. We computed the proportion of each client type from the study facilities in the NASCOP data and estimated the average number of VL tests per month per client.
-
Expected amount of ART and other pharmaceuticals needed per month, by facility: For this activity, we based the quantity on cotrimoxazole—an antibiotic commonly prescribed for PLHIV—and the most commonly prescribed ART (TDF-3TC-EFV). About half of patients also need TB prevention drugs (INH and Pyridoxine). We calculated the total amount of these pharmaceuticals needed per ART client per month in kilograms based on every client requiring a one-month supply of CTX and TDF-3TC-EFV, and half of clients requiring a one-month supply of TB drugs.
-
Minimum number of VL testing days required by each facility every month: Collapsing the number of days when VL tests are offered for any one facility will reduce the number of trips a UAV must make to each facility. Using the NASCOP data, we identified the maximum number of tests per day conducted by each facility between January and March 2018 and consulted with the Afya staff to determine the appropriate maximum number of clients the average facility could offer VL testing services for in one day.
Modeling the current transportation system
We extrapolated the number of trips taken per facility to deliver VL samples to Lodwar from facility logs and then to Eldoret and pick up ARVs during the January to March 2018 quarter to provide a basis for estimating the annual ground-based transportation costs. This time frame was chosen to reflect the practices, costs, and targets achieved without the externally funded Afya program, which, through interventions to fund the transportation of VL samples, is reducing costs and improving service delivery. These annual costs for transportation of VL samples and ARVs were compared to the annual costs derived from modeling the UAV-based scenarios.
Designing the UAV scenarios
Based on these assumptions, four scenarios (Table 3) were created that partially or fully replace the ground-based transportation network with a single UAV. All scenarios prioritize the transportation of VL samples, and some include UAV transportation of ARVs.
The scenarios differ by changing the settings of three parameters:
-
The number of health facilities where the UAV lands to pick up VL samples and drop off ARVs
-
The UAV partially or fully supporting the pick-up of VL samples to transport to Lodwar
-
The UAV partially, fully, or not at all supporting delivery of ARVs to health facilities
These parameters were chosen as they could impact the total UAV operational time, and thus the UAV costs. Exclusively transporting VL samples, picking up VL samples from centralized hub facilities instead of each facility, and delivering limited supplies of ARVs could all impact cost and TAT-1. All UAV models include the transport of VL samples from Lodwar to Eldoret by UAV.
Modeling the UAV scenarios
We produced a one-month schedule that reflects the average needs for VL sample transport and ARV delivery per facility for each scenario. For each week, the schedule begins with the UAV delivering ARVs and picking up VL samples on Tuesday morning from facilities that provided VL testing services on Monday. The samples are warehoused at Lodwar each day until they are flown to the lab in Eldoret. This allows facilities to provide VL testing starting Monday, then Tuesday through Thursday for pick up by UAV, and Friday (or earlier) as the day this UAV transports all VL samples to Eldoret. Additionally, this scheduling should allow the TAT-1 to stay within the target. We temporally grouped UAV trips to facilities in the same area so that the UAV could make multiple stops in one trip, when distances allowed. We calculated the total weight in kilograms of deliveries and pickups per week for each facility.
Next, the weekly trip calculations were loaded into the Vehicle Routing Problem (VRP) solver in ArcGIS, which recognized the quantities of materials to transport from one location to another. Using the UAV flight path network, the tool was configured such that the UAV would travel from the base at Lodwar with the maximum payload weight to as many health facilities in one trip as possible and return to Lodwar once one or more of the constraints were met: maximum UAV distance on one tank of fuel, maximum operating time, or end of operational hours at the facilities. The UAV is modeled to land at its first health facility, have the ARV payload removed and have that facility’s VL samples loaded within the maximum payload weight constraint. Depending on the scenario, the UAV may fly to more health facilities to pick up VL samples, returning to Lodwar once the weight constraint was met. If enough time remained in the same day to take additional trips, the UAV would refuel as needed and conduct another trip. The VRP solver would repeat this process until all trips were accomplished for that week.
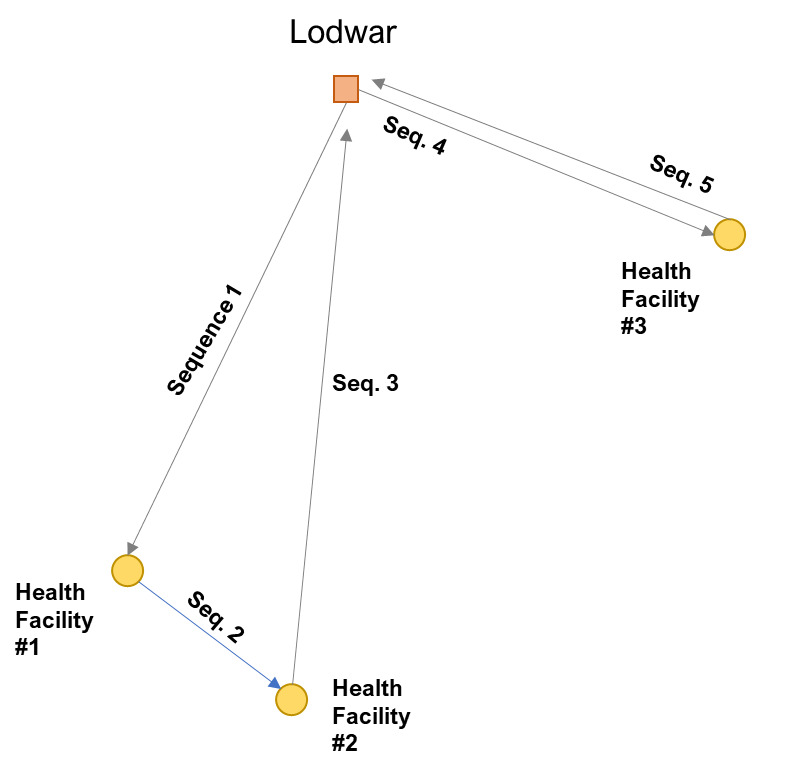
The product of the VRP solver is a database of “sequences,” providing the routes, travel times, payload delivered, and payload picked up for every trip. Figure 1, an illustrative example, shows these sequences, and how the resulting product could create a trip with multiple stops (sequences 1, 2, and 3), or a trip to only one facility and back to Lodwar (sequences 4 and 5). A solution was generated for every week for the generic one-month period. We summarized these flight sequences to calculate the total operational time (i.e., time spent preparing the UAV for flight, loading and unloading at the UAV base, refueling, flight time, and time spent loading and unloading at health facilities) per month for each scenario. This total time was used to calculate UAV costs annually. To these costs, we added any additional ground-based transportation costs using the known fare, box surcharge, and per diem rates earned by facility staff when away from facility.
RESULTS
Data on the number of trips undertaken to transport VL samples between January and March 2018 was available for 11 of the 15 facilities. For the four facilities where no information was collected, only one was found in the NASCOP database to show it had sent samples. Therefore, 12 of the 15 facilities conducted VL testing in this quarter. According to the health facility transportation logbook records from January to March 2018, health care workers took 63 total trips from 12 facilities, carrying between 1 and 35 VL samples per trip. (Data discrepancies exist between the NASCOP data and the health care logbooks for most facilities.) The latest available data from NASCOP (September 2017) showed 1,316 ART clients in care at these facilities (average = 87.7 clients per facility; range = 3 to 231).
The calculated values for the variables included in the models are listed in Table 2. Based on these data and conversations with the Afya staff, we estimated that one ART client would require 0.1 VL samples per month and 0.2 kilograms of ARVs per month, and that the average facility would provide a minimum of one VL testing day per month for up to 10 ART clients. To generate monthly totals for VL samples and ARVs by facility, these values were multiplied by the number of ART patients at each facility. All costs are listed in US dollars (USD), and costs originally provided in Kenyan shillings (KSH) were converted to USD where 100 KSH = 1 USD.
Based on these data and optimal routing, we modeled the four UAV-modified scenarios and estimated TAT-1 and cost, which are compared to the current configuration model (Table 4).
Results of the current system
We estimated the annual cost to transport all VL samples from health facilities to the laboratory in Eldoret, and to transport ARVs from Lodwar to each health facility to total US$56,350/Ksh5,635,000. Only 3% of the VL samples met the TAT-1 goal of under four days. To provide an annual cost, we assume the same number of VL sample trips and trips to pick up ARVs that happened between January and March 2018 will happen for the rest of the year. Only the 12 facilities that recorded sending VL samples in their logbooks between January and March 2018 are included in this scenario. No data were collected on the trips health care workers took to retrieve ARVs from Lodwar and were assumed that one trip per facility was taken each month, incurring the average fares and surcharges for carrying boxes. Based on conversations with providers we estimated that each trip took providers away from their facilities from between one-and-a-half and two days.
UAV-based scenario results
Scenario 1: In this scenario, UAVs completely replace ground-based transportation of VL samples by landing at all facilities at least once per month to pick up the samples and take them to Lodwar. No ARVs or other supplies are carried by UAVs, meaning health workers still need to travel to Lodwar to pick them up. The estimated annual cost for this model is US$172,878/Ksh17,287,800 which is 3.1 times the cost of the current system and is inclusive of the trips health care workers would have to take to pick up ARVs from Lodwar. While all VL samples would reach the lab in under four days, all health facilities would still see similar rates of staff being unavailable as they travel to Lodwar to pick up ARVs.
Scenario 2: This scenario builds on Scenario 1 by adding partial distribution of ARVs via UAV. Under this scenario, the UAV lands at every facility, delivering 10 kilograms of ARVs to each facility for every trip taken to pick up VL samples (except in two instances where the UAV lands at one of two neighboring facilities; in that case only one of the facilities would receive the package per delivery). After delivery of ARVs, the UAV picks up VL samples and returns to Lodwar. For Scenario 2, the estimated cost is US$183,363/Ksh18,336,300 or 3.3 times the current costs. All VL samples would reach Eldoret in under four days, but health care workers from all but two facilities would still be required to travel once a month to Lodwar to pick up ARVs that were not transported by the UAV because it could not carry all required ARVs.
Scenario 3: In this scenario, the UAV lands only at four “hub” facilities and three other facilities that are too remote to travel to a hub or to Lodwar easily. Facilities where the UAV does not land are required to travel to their closest hub via ground-based transport. Facilities that were within 20 km from other facilities were considered part of a hub system and the facility with the most ART clients in each system was chosen as the hub. In one instance, a facility was within 10km of a hub, but the road network used to reach the hub was significantly challenging such that it was considered a remote site. Only hub or remote sites would receive one 10kg package of ARVs per VL trip, but all sites would have their VL samples ultimately transported to Lodwar from the hub using the UAV. Two facilities were able to receive all ARVs this way, but the other facilities still required health workers to travel once per month to Lodwar to get their month’s supply of ARVs.
Reducing the number of landing sites could reduce costs, however as the UAV lands at four hubs and three remote sites in this scenario, the costs are similar to previous scenarios. Eight sites would still have to use ground transportation to reach their UAV hub, and all sites would still require staff to travel to Lodwar to pick up all their ARVs. The cost, including additional ground-based transport is US$179,401/Ksh17,940,100 or 3.2 times the current costs.
Scenario 4: The UAV completely replaces the ground-based distribution network of ARVs from Lodwar to each facility and includes the transportation of all VL tests from each site to Lodwar. The number of flights per month is based on the amount of ARVs required as more flights are needed to transport ARVs than are to pick up VL tests. Seven facilities require only one UAV trip per month to pick up all VL samples and deliver all needed ARVs, while eight facilities will be visited by the UAV an additional one to two times per month compared to what is needed to pick up VL samples only. Health care workers would not need to travel for ARVs, increasing their availability at the clinic. This cost, however, is the highest, at US$200,208/Ksh20,020,800 or 3.6 times the current amount.
Because of the increased demand on a single UAV, during two of the four weeks the UAV would have to fly to Eldoret on the following Saturday, which means the batch of VL samples it transported from the facilities visited on Tuesday and housed at Lodwar would not reach Eldoret for five days, two days beyond the TAT-1 goal.
DISCUSSION
In our modeled scenarios, using a UAV reduces the first segment of turnaround time of VL samples while increasing coverage to the 95% target achieving key goals in this region. Additionally, when providers are not responsible for the transport of samples, use of UAVs ensures that health care providers are not taken away from their duties to transport samples for one to two days a month. The opportunity costs of using health care providers for transporting samples are not included in these models but are estimated to be considerable especially given shortages of trained health workers are common in Kenya and Turkana in particular.
However, using UAVs to transport VL samples in Turkana County would be significantly more expensive than the current ground-based transportation system. The least expensive UAV scenario is still more than three times the cost of the current system and the current costs of ground-based transportation are already high in Turkana. When compared to facilities in the more densely populated Siaya County, Kenya, (the only county with available data on transportation costs for VL samples in Kenya) the ground-based transportation cost for 4,377 VL samples (DBS and whole blood) totaled US$53,294/Ksh5,329,400 in 2014—approximately double the number of samples for about the same transport cost.24 However, the price of the UAV and the subsequent hourly rate charged by the logistics company operating the UAV will likely decrease as manufacturers’ costs decrease over time, a common trend with any emerging technology. Additionally, expanding the use of UAVs to cover transport of more items than included in the modeling in this paper may also help reduce costs.
While UAVs are currently cost-prohibitive under this model, they could become more cost-competitive over time if the technology proves successful and costs are reduced. Other aspects of systems-level feasibility should also be considered. For the UAV configurations to work as modeled, each facility must consolidate their VL testing schedule to aggregate client visits for VL testing to specific days so that the UAV can land at multiple sites on the same day. This would likely require central coordination, which may incur more costs. As a scrub desert with low population density and limited infrastructure such as power lines or tall buildings, Turkana is an excellent location for a UAV program. While weather related issues must be considered before the development of a UAV program, these did not present a critical problem for the type of UAV used for modeling. Additionally, a UAV would likely not be affected by the same factors that currently limit ground-based transport (e.g., community violence, road bandits, roads closed from flooding) and may provide an alternative that offers continual, routine transportation solutions.
While reducing the number of days when VL tests are collected improves efficiency when using UAVs and decreases TAT, this practice could complicate patient care as clients in large and rural areas currently struggle with travel to facilities. If transportation is a challenge, then it is also probably difficult for patients to reach facilities. Unless facilities are able to see all patients on these VL testing days, that means asking patients to possibly make multiple trips, thus transferring the burden from the health system to the patient. Also, in some places, health systems are moving away from ART clinic days, and are instead integrating HIV treatment into general outpatient services to reduce stigma. In light of this, implementing specific VL testing days just to accommodate UAV transport, may be a problematic approach.
We recognize this modeling activity has several limitations. Our scenarios are focused on transporting VL samples and to varying degrees ARVs, but EID and TB tests are also important laboratory samples that require transportation. EID tests are required to be taken to a laboratory within a day of the birth of a child and returned to the health center as soon as possible and were not included in our model for this reason. To keep this timeframe even when a UAV is fully utilized for VL sample transport, staff may still have to use ground-based transportation. However, EID samples could easily fit on the UAV if the timing was appropriate. TB sputum specimens require more space, more rapid transport and must be kept at a constant cold temperature, complicating transport by UAV unless those UAVs are designed specifically to do so.
Finally, our estimated UAV costs come from one company which may not reflect charged by other providers. However, while other logistics companies may have similar plans to add UAVs to their fleets, we believed this company’s understanding of the UAV landscape and local regulations, as well as their involvement in Turkana made them an ideal source. We also relied on this company to provide the estimated specifications of an aircraft they are considering purchasing once on the market and to vet the UAV manufacturer. The logistics company indicated the UAV model used in this activity was the best fit for the distances and payload required. Our modeling provides a first glimpse on the cost and design of a UAV-augmented laboratory transport system. While our results provide an estimate of the costs of UAV assisted lab transport given the best data available at the time, we also acknowledge rapid changes to UAV technology will impact the cost and time of transport. Finally, once the technology is available, additional costs including operation and maintenance, program oversight, and training must also be considered.
CONCLUSIONS
Increasing the number of ART clients who are virally suppressed to reach the 95-95-95 goals requires establishing and maintaining connections between health facilities in remote areas and laboratories and commodity storehouses. Introduction of UAVs into the HIV supply chain for facilities in this study could reduce the turnaround time for VL samples and support positive health outcomes for the ART clients. However, using current, Turkana-specific cost estimates, UAVs are not cost competitive with the current ground-based transportation system as we have modeled in these scenarios, and the practice of consolidating VL testing days to accommodate UAVs may not be practical for patient care. As costs decrease and technology improves to allow for increases in carrying capacity and the distance that it can travel before refueling, as well as more frequent flights, a UAV-modified transportation system for VL samples and ARVs may one day be logistically and financially feasible for Turkana.
Acknowledgments
The authors would like to thank the Turkana County, Kenya Health Department for their important support of this work.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authorship Contributions:
CP ([email protected]): Conceptualization; data curation; formal analysis; investigation; methodology; project administration; resources; software; visualization; writing original draft.
EE ([email protected]): Conceptualization, funding acquisition, investigation, methodology, writing original and draft, writing review and editing.
KS ([email protected]): Conceptualization, methodology, validation, writing review and editing.
ME ([email protected]): Conceptualization, funding acquisition, methodology, writing review and editing.
RH ([email protected]): Methodology, writing review and editing.
ML ([email protected]): Methodology, writing review and editing.
DO ([email protected]): Investigation, writing review and editing.
Competing interests
The authors completed the Unified Competing Interest form at www.icmje.org/disclosure-of-interest/ (available upon request from the corresponding author), and declare no conflicts of interest.
Correspondence to:
Emily Evens, PhD, MPH
FHI 360 359 Blackwell Street, Suite 200 Durham, NC 27701, USA