Pneumonia remains to be one of the major public health concerns that cause childhood morbidity and mortality worldwide. 1 Globally, 920,000 pneumonia cases led to childhood deaths, of which 80 percent occurred in the first two years of life and majority of these cases occurred in the world’s poorest regions with highest incidence in Sub-Saharan Africa and South Asia. 2,3 Although substantial progress has been made in reducing under 5-year old child mortality resulting from the launch of UN Millennium Developmental Goals 4 (MDG 4), childhood pneumonia still ranks as the leading cause of childhood mortality, thus remains a challenge in the Philippines. 4,5
It is estimated that close to 4.5 million cases of suspected pneumonia do not receive care from an appropriate health provider. 6 Appropriate health seeking behavior reduces the potential occurrence of severe and life-threatening childhood illnesses, specifically pneumonia. 7 Household poverty emerged as the primary determinant in shaping health-seeking behavior. 8,9 Previous studies found that those poor families, especially in rural communities, delay or deter consultation to healthcare facilities because of the costs of hospitalization and their poor recognition of signs and symptoms. 8
Rural households preferred home treatments during the early stages of an episode of acute respiratory infection (ARI) through the use of conventional and western medicines, use of homemade or purchased herbs and use of previous prescriptions. 10–13 The prevalence of self-medication in managing ARI episodes is very high in both developed and developing countries, and varied significantly with a number of socio-demographic characteristics. 14 Several caregivers were reported to have alarming rates of self-medication with western medicines, 15,16 with antibiotics used as a panacea for childhood illnesses. 17,18
Numerous studies have shown that illness symptoms and perceived severity; children’s and mothers’ age, caregivers’ education, and total family income are strongly associated with care seeking behavior. 7,19–21 Distance, travel time to the health facility, costs of care, and service availability are also important determinants of seeking care. 5,22 However, there is a dearth of current information on health seeking behavior and medication use in response to ARI episodes in the Philippines.
This study was designed to describe patterns of health seeking behavior taken by caregivers of children under five years old in response to ARI episodes as well its determinants. The findings of this study may provide better understanding of ARI related health seeking behavior and medication practices to improve current efforts to reduce childhood pneumonia morbidity and mortality and develop supplementary strategies for the delivery of control programs.
MATERIALS AND METHODS
Study site
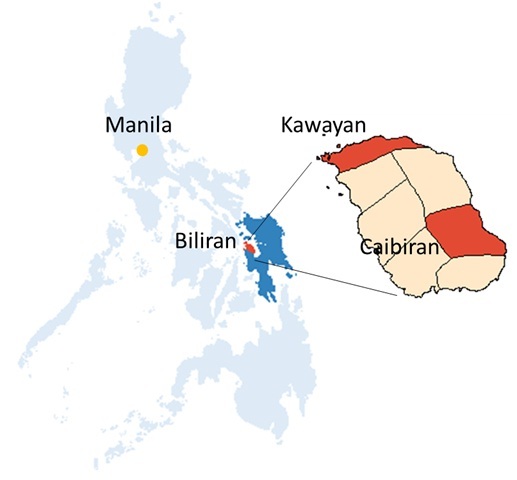
This paper is part of a larger study that looked into Acute Respiratory Infections in children. 23 A prospective cohort study was conducted in Biliran, an island province located between the islands of Leyte and Samar in the Eastern Visayas region in the Philippines, with a total population of 161,760. 24 It is classified as a fourth-class province, with a predominantly agriculture and fishery economy and is considered as one of the poorest provinces in the country. It was chosen as the study site due to its relatively stable population migration patterns and simple health referral system. 23 The map in Figure 1 shows locations of municipalities of Kawayan and Caibiran, where the study took place. Based on the results of a rapid assessment study, 5 the expected incidence of childhood pneumonia/year and severe pneumonia/year are 400 and 250, respectively. The study enrolled 2,500 children under five years old who were residents of 15 barangays in Kawayan and 10 barangays in Caibiran.
Study procedures
Written Informed consent was obtained from parents of children under five years old who agreed to be included in the study. Socio-demographic information was gathered for each household member using questionnaires in the community’s native dialect; caregivers were taught to fill out calendars (called “disease calendar”. See Figure S1 in the Online Supplementary Document) where they recorded presence/absence of respiratory signs and symptoms they observed in their children on a daily basis and the action they took in response to them. These signs and symptoms included cough, nasal congestion or runny nose, difficulty of breathing, rapid breathing, chest-in-drawing and general danger signs such as inability to feed or vomiting, lethargy, and convulsion. A nurse visited the households every two weeks and inspected the disease calendar for completeness; if there were no or incomplete entries in the calendar, the nurse guided the caregiver to completely fill it out by recalling information. If there were entries in the disease calendar, the nurse confirmed them. A tablet Personal Computer containing a video of a child with rapid breathing and chest in-drawing was shown to the caregiver to facilitate the validation of those symptoms. Forms and procedures were pilot-tested prior to the actual conduct of the study. Households with newborns in the study sites were asked to participate in the study and children who reached five years old were removed from the cohort. The information from the disease calendar was encoded into a database.
Case and operational definitions
Clinical signs of ARI recorded in the disease calendar were put together and categorized based on the Integrated Management of Childhood Illnesses (IMCI) guidelines 25 with some modifications. Cough or colds without any other signs of respiratory illness was categorized as cough or colds; the presence of difficulty of breathing with cough was categorized as a pneumonia case. Severe pneumonia in the IMCI classification was divided into two: pneumonia cases with chest in-drawing were categorized as chest in-drawing pneumonia (CIP), while very severe pneumonia (VSP) included children with pneumonia and or CIP and with any of the following symptoms: convulsions, inability to eat or drink, inability to wake and/or vomits everything. A new episode is the presentation of ARI signs and symptoms after being symptom free for seven days. The duration of the illness was calculated based on the first appearance of a respiratory symptom and disappearance of all symptoms. When there is a progression of the child’s illness based on the signs and symptoms recorded, the more severe IMCI classification was used.
The actions taken by the caregiver in response to an ARI episode were categorized into the following: (a) no action taken, (b) health facility consultation and (c) self-medication. Health facility consultations involved referrals or consultations to any formal health facility, which includes the Biliran Provincial Hospital (BPH), Rural Health Unit (RHU), Barangay Health Station (BHS), and private clinics. The BHS is the first level of primary care in the Philippine Health System while the RHU is the first level referral for BHS. The BHS is usually managed by a midwife and Barangay Health Workers (BHWs) while a doctor, nurse and other medical personnel are stationed at the RHU. 26 Self-medication is the use and administration to the child of medicine, without health facility consultation. This included western medicines, antibiotics and traditional medicine. Traditional medicine involves the use of herbal preparations or seeking advice from traditional healers. Western medicines are treatments to medical conditions developed through scientific methods such as antipyretics and bronchodilator (Supplemental Table 1). No action was considered as the least appropriate response followed by self-medication, while health facility consultation was the most appropriate. We used the more appropriate action taken during the illness episode when there were multiple actions.
Socio-economic status was estimated using a 10-item index developed and validated by Schreiner specifically for the Philippines. 27 A score is calculated to determine the poverty level of the household in relation to the poverty line. The self-medication rate (SMR) was calculated by dividing the number of ARI and pneumonia episodes which used medicine without prescription for a current illness episode by the total number of ARI and pneumonia episodes.
Data analysis
Univariate analysis was done to identify possible determinants for self-medication as well as inaction for a pneumonia episode regardless of severity, with a screening criteria of p-value less than or equal to 0.25. Multivariate multinomial logistic regression was then applied. Explanatory variables in final model were selected by backward stepwise method with an exit criteria of p-value less than or equal to 0.05. Odd ratios (OR) and 95% confidence intervals (CI) were calculated. Analyses were performed using STATA statistical software (Stata Corp, College Station, TX, USA) and R 3.5.0 (R Development Core Team, Vienna, Austria).
RESULTS
Socio-demographic profile of the caregivers
A total of 3,056 children under five years old were enrolled in the cohort and visited from February 2014 to June 2015. Majority of the primary caregivers were mothers (84%), while the rest were fathers or other relatives. Less than half (44.9%) of the caregivers were between 21-30 years old (mean: 31.9 years old; SD±10.4); 52% had high school education, or an equivalent of 10-12 years of schooling. Median size of the households was 6 with a range of 2 to 22, with about one fifth of households having an income below the poverty line of US$ 0.71 or PHP 39.52 per person per day based on the 2003 Family Income and Expenditure Survey (FIES). 27 Of the 3,056 children, 97.1% had at least one ARI episode (range of 1 to 21 episodes) and 142 children had at least one pneumonia episode (range of 1 to 7 episodes). There were 15,796 recorded episodes of ARI in the period (Table 1). Nearly all of the ARI were cough or colds (98.8%), whereas there were 191 episodes of pneumonia, CIP and VSP. About half of pneumonia episodes were experienced by children aged ≤2 years old (48.2%) and more males than females had pneumonia (58.1% vs. 41.9%). For illness episodes that progressed to pneumonia, it took an average of 6.59 days (SD±17.2) before the manifestation of difficulty of breathing or chest in-drawing.
Patterns of health seeking behavior
A large proportion of caregivers did not take any initial action when the child had cough or colds. Of the 191 pneumonia cases, caregivers brought 53.4% of them to health care facilities. The RHU was most frequently sought source of care regardless of category (Table S1 in the Online Supplementary Document). Only few of the cases were brought to the BHS (2.1%), and the private clinics (5.8%). In terms of the timing of visiting a health facility, 26.7% of pneumonia cases were brought on the same day when a case developed signs. Proportions of cases who were brought to health facilities on the same day were 24.3% and 37.5% in pneumonia and CIP respectively while it was 27.3% in VSP. A quarter of caregivers did not take any action on that day (26.2%). Self-medication was practiced in 47.1% for all pneumonia cases. Overall, 12.6% used antibiotics without prescription from any health care worker. On the average, a pneumonia case was brought to a health facility 1.2 days (SD±4.4) after the appearance of difficulty of breathing or chest in-drawing. It ranged from the day of appearance of symptoms to 37 days after. On the other hand, for cases that were not brought to a health facility on the day the symptoms first appeared, it took an average of 2.8 days (SD±5.4) after the onset before the consultation took place.
Self-medication rate (SMR) for all forms of pneumonia was 38.0%, highest among the pneumonia cases and lowest in VSP (Table 2). The rate was almost stable between age groups whilst increasing along with age among pneumonia and CIP cases. Rates of antibiotic use was slightly higher in all forms of pneumonia than the cough or cold cases (Table S2 in the Online Supplementary Material). On the average, caregivers used two types of medicine for pneumonia while one type of medicine for cough and colds episodes. Table 3 shows the number of subsequent actions taken after administrating self-medication among any pneumonia forms. Subsequent actions of caregivers of pneumonia cases showed that a large proportion eventually went to a health facility during the course of the illness episode.
Determinants of health seeking behavior
There were no determinants associated with self-medication of medicines other than antibiotics for pneumonia episodes (Table 5). The odds of antibiotic self-medication in households with 2 or more children were higher than in households with only 1 child. Also the age of the child at the time of the ARI episode was associated with not taking action during a pneumonia episode.
DISCUSSION
Our findings revealed that children in rural areas have fewer episodes of pneumonia regardless of disease severity compared to previously reported estimates. The data showed that the percentage of children having pneumonia to VSP is only 1.2%, lower than the 10.6% recalculated from a cross-sectional study in the same locale 5 and prospective population-based surveys of Hortal, et al 28 in Uruguay, Thörn et al., in Brazil 29 and le Roux et al., in South Africa. 30 Our findings were rather similar to the estimates in the 2013 Philippine National Demographic Health Survey (PNDHS) where rates of prevalence for ARI among children under five years of age in the past two weeks was 6%. 31 The conflicting findings with the previous study 5 can partly be attributed to the difference in methodological designs. The study derived ARI prevalence from a single question with a recall period of 1 year. We used self-diary in the cohort to record ARI episodes with which pneumonia was classified from signs and symptoms that has been checked every two weeks. Our calculation could give more accurate pneumonia prevalence estimate since recall bias could have been minimized.
Appropriate health seeking behavior is critical to the reduction of childhood deaths. In fact, several studies reported that the delay could lead to complications resulting to less effective medical care. 21,32 The community patterns in response to pneumonia episode in this study implicates that caregivers may appear to recognize signs of illness early in the episode but inappropriately responded to them. Our results also showed that half of the pneumonia cases were brought to health facilities, and 47% either took no action or resorted to self-medication. This is somewhat comparable with the PNDHS report that more than half of the (64%) of children with ARI were taken to a health facility or a health provider and half of children with ARI received antibiotics. 31 The survey results were slightly higher partially due to accounting actions for ARI in addition to pneumonia. We also highlighted a certain number of self-medication with western medicines in response to ARI episodes as described in some studies. 10,13 Moreover, the actions taken were highly dependent on the presenting symptoms. Hardon noted that initially if children did have cough and colds without accompanying fever, they opted to resort first to herbal preparations instead, such as Kalamansi (lime) juice in urban slum areas in the Philippines. 33 Fever was a notable indicator that the condition is severe and needs medical attention. 33 This is incongruent with the study performed in Bohol, Philippines where it was reported that the low utilization of health facilities resulted from complex assumptions and indigenous explanatory model on ARI illness that the parents hold. The consultation pathways were triggered by the perceived cause of cough (if cough is due to wind, due to change in weather, or due to a sprain) and caregivers’ perception of the severity of the cough. Specific actions or necessary treatments of caregivers were highly dependent on continuous reassessment of cause and symptom, in turn resulting to delays in health facility utilization. 10 Further, the timing of the decision to seek care to health facility was broadly dependent on mothers’ and family’s understanding of the severity of the child’s condition. 6,18–20,33
Our study also found out that having 2 or more children under five years old in the household was associated with antibiotics self-medication and that the caregiver of a child less than 1.5 years of age was less likely to do no action during a pneumonia episode. The finding concurs with a study conducted in the communities of Nigeria, Ethiopia and Democratic Republic of Congo. 34 Although there was no reported significant association to other socio-demographic characteristics such as child’s gender, location, and number of symptoms dissimilar from other reports, 5,28,32,35,36 this informs the need to strengthen efforts on educating caregivers on the signs and symptoms, the severity of the ARI episodes, and on when and where to immediately take the child to the health facility. The reason for this disparity is not clear but suggests that it was probably due to the variances in methodologies (different approach in data collection, study population, cultural differences and locale of the study).
Self-medication was observed to be more frequently taken as a first action. We also noted that while 68% of pneumonia cases self-medicate as their first action, 53% eventually seek health facility consultation. In a study of Myanmar mothers, inappropriate practice of self-medication with western medicines was found to be frequently utilized followed by indigenous and traditional medicines. 15 Our findings also highlight the alarming rate of self-medication with antibiotics and unnecessary polypharmacy in response to ARI episodes across disease severity as described in a couple of studies done in rural communities of Vietnam, where mothers used antibiotics as if such drugs were panacea. 18,36 Antibiotics are the most widely used category of drugs because they are readily available and because bacterial and viral infections have common manifestations. 37 Overuse and misuse of antibiotics was particularly high (50% to almost 100%) in upper respiratory infections, most of which are generally viral and self-limited. A study conducted in the Philippines underscored that 86% of mothers in rural communities of northern Mindanao responded to ARI episodes by giving home medications, such as purchase of antipyretics at sari-sari (local grocery shops) stores, the use of prescriptions from past illness episodes, and the use of herbs. 12 Lansang et al. also reported that the use of antibiotics was recognized as “vitamins” or as “first aid” prior to medical advice, and more than half of which were purchased without prescription. 17 Kim et al. also confirmed that children with ARI symptoms in an urban community in the Philippines were self-treated with Amoxicillin or its derivatives, Cotrimoxazole and Cephalosporins. 38 Further, Planta emphasized that the irrational use of antibiotics without proper diagnosis of the disease leads to emergence of multiple resistant strains of the causative organisms, which in turn, are difficult and costly to treat, especially for immune-compromised individuals. 39 In this regard, our results suggest that improved rational drug use should be made as a strategy to reduce inappropriate antibiotics use for ARI episodes in the Philippines.
Identifying pneumonia cases and instituting appropriate antibiotic therapy is still the primary strategy in reducing pneumonia morbidity and mortality in the Philippines. The strategy is under the Care for the Respiratory Infections (CARI) program of the Department of Health where IMCI strategy is being utilized. 40 It is a simple strategy that is intended to guide decisions on referral, antibiotics therapy, need for oxygen and intensity of monitoring, thus offering a system of prioritizing and rationalizing resource use. 41 However, Bhutta (2006) raised the concern that the existing diagnostic criteria can lead to significant overtreatment of children with respiratory infections. 42 And once the treatment went to the hands of the community health workers, there is actually a large-scale threat on drug misuse and over use and risk of the development of drug resistance. 1,43 On that note, the WHO released the revised classification and treatment for childhood pneumonia at first level health facility and outpatient department, which simplifies the management and treatment options, and to reduce the number of referrals for hospitalization, 44 and this update is currently being discussed and reviewed for local adaptation in the Philippines. The current state of IMCI program of DOH should be reviewed to find out if this strategy is working in the country.
Greater focus on local health staff empowerment and capacity building is imperative to ensure that proper diagnosis and management of cases is being delivered in the communities. There is a need to strengthen the delivery of health education focusing on promotion of responsible use of antibiotics and identification of danger signs of ARI to improve appropriate health seeking behavior of the caregivers. Finally, different techniques of the delivery of information should be explored to amplify its reach and acceptability in the local settings.
Limitations and future research
One limitation of the study is that it was largely based on the self-reported behavioral practices using a two-week recall period. Although nurses confirmed the information, these could have been subject to recall bias and underreporting of cases. However, the biases were reduced through nurses’ frequent visits to the household. The nurses validated the recordings, and if there were inconsistencies, caregivers were requested to record it in the presence of the nurses so that they will record it correctly. By virtue, caregivers were encouraged to be more compliant and made them realize the importance of the proper recording. Additional research is needed to more closely examine the determinants in health seeking behavior.
CONCLUSION
Overall, these findings suggest that there was inappropriateness and delay in seeking care to childhood pneumonia in rural areas. Our determinants are number of children under 5 years old and age at the time of episode. All of these factors should be taken into consideration when designing health policy and intervention programs to reduce morbidity and mortality cases of childhood pneumonia.
Acknowledgments: We would like to acknowledge and thank the partners, health officers, caregivers and field staff in Caibiran and Kawayan municipalities, and health officers of Biliran province, Philippines.
Disclaimers: This publication reflects only the authors’ views, and the European Union is not liable for any use that may be made of the information contained herein.
Ethics: This study was reviewed and approved both by the Ethics Committee in Tohoku University Graduate School of Medicine and the Institutional Review Board of the Research Institute for Tropical Medicine of the Philippines.
Funding: This work was supported by Japan Science and Technology Agency and Japan International Cooperation Agency, Science and Technology Research Partnership for Sustainable Development and Science and Technology Research Partnership for Sustainable Development Japan Initiative for Global Research Network (J-GRID) from Japan Agency for Medical Research and Development (AMED) under Grant number JP15fm0108013. The funders had no role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Authorship contributions: Conceived and conceptualized the study: MDR, RT, AT, TK, PA, JL, VT, HO. Conducted data analysis and performed data interpretation: MDR, RT, AT, TK, HO. Prepared the initial draft of the manuscript: MDR, AT, TK and RT, VT, HO contributed to the report writing and critically reviewed the manuscript.
Competing interests: The authors declare no conflict of interest. The authors have completed the Unified Competing Interest form at www.icmje.org/coi_disclosure.pdf (available on request from the corresponding author) and declare no conflicts of interest.
Correspondence to:
Mark Donald C. Reñosa
Senior Science Research Specialist
Department of Epidemiology and Biostatistics, Research Institute for Tropical Medicine
Filinvest Corporate City
Alabang Muntinlupa City
Manila
Philippines 1781
[email protected]